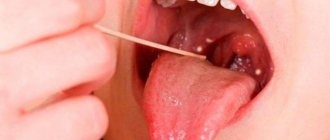
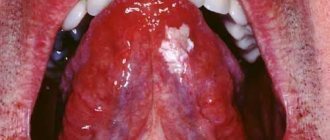
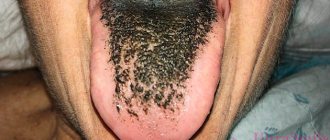
We are used to the fact that we need to go to the dentist if we have problems with our teeth or gums. What to do if you have inflammation of the tongue or glossitis? Dentists identify more than 10 types and subtypes of infection. The infection can be caused by both fungus and bacteria. Viral infection is less common. Inflammation can be caused by a lack of certain vitamins and minerals, or hormonal changes. There are many reasons for the disease, so it is important to identify what exactly caused the inflammatory process.
Causes of glossitis
- improper oral hygiene;
- bacterial infection;
- fungal infection;
- heavy metal poisoning;
- bad habits (smoking, alcoholism);
- congenital pathologies of the tongue (folded tongue);
- allergic reaction;
- tongue injury (often caused by malocclusion);
- oral infections;
- lack of iron in the body;
- burn of the mucous membrane (hot food or drinks);
- infectious diseases (AIDS, tuberculosis, scarlet fever, measles).
Pain on the tip of the tongue
There may be several reasons for the occurrence of such pain:
- Mini tip injury . In first place in terms of prevalence are mini-injuries of the tip of the tongue. Most often, patients inadvertently bite the tip of their tongue or burn it with too hot food. Such mini-injuries are painful and cause a lot of trouble for patients; the papillae hurt, and sometimes eating becomes impossible for a while due to severe pain. Over time, everything heals and passes without a trace.
- Glossalgia is a serious disease in which the tip of the tongue most often hurts, less often its sides. The pain is manifested by a burning sensation; patients often complain that their tongue hurts, like after a burn. Sometimes the painful sensations spread to other organs of the oral cavity; the patient’s tongue and gums, sometimes lips and cheeks, hurt. If such symptoms are detected, you should immediately consult a doctor, since glossalgia is difficult to treat and exhausts the patient with its symptoms.
- Glossitis is an inflammatory disease of the tongue. When it occurs, the tip of the tongue can be very painful, because the infection that causes inflammation usually gets into the wound, and the tip of the tongue is bitten much more often than other parts of it.
- Stomatitis is also accompanied by severe pain in the tongue, which becomes covered with painful ulcers located over its entire surface.
- Allergy . Allergic reactions are also common causes of pain.
The most common types of glossitis
The most common occurrences in dental practice are:
- acute catarrhal glossitis;
- tongue abscess;
- desquamative glossitis.
Acute catarrhal glossitis is the most common type of inflammation. Inflammation can be caused by microbes or mechanical damage to the tongue. The predominant symptoms are pain, redness and swelling.
A tongue abscess is the appearance of an abscess in the tongue. The abscess can be superficial, under the mucous membrane, or maybe in the thickness of the tongue. Abscesses in the thickness of the tongue, in addition to pain in the tongue, can cause a disturbance in the general condition. A person develops a fever, a headache, and weakness. Most often occurs due to injury to the tongue.
Desquamative glossitis, also known as “geographic tongue,” most often appears in children. It appears in the form of various spots on the tongue, which look like a white coating, alternating with areas of pink mucous membrane. There are no changes other than appearance. Scientists have identified a clear reason for it. The main factors are believed to be bacteria, allergic reactions and hormonal imbalances.
Sore throat: possible causes, diagnosis and treatment
Sore throat is a common complaint of patients when visiting an otolaryngologist, therapist, pediatrician and general practitioner. The causes of sore throat can be infectious and inflammatory diseases of bacterial and viral etiology, inflammatory processes in the pharynx, larynx and surrounding organs caused by non-infectious factors, and non-infectious pathology (
). Before proceeding with pharyngoscopy, it is necessary to carefully detail the patient’s complaints and collect an anamnesis. The patient can call a sore throat the unpleasant sensations of scratching, burning, soreness, rawness, the feeling of a “foreign body,” the intensity of which is conveniently assessed on a 10-point scale, where the maximum manifestation of pain is rated at 10 points, the minimum at 1 point.
It is important to determine what, in the patient’s opinion, preceded the onset of pain and what other symptoms it is accompanied by. If there is hyperthermia, then the inflammatory nature of the disease is most likely: pharyngitis, tonsillitis (tonsillitis) [16]. Refusal of food and water can provoke severe pain in aphthous stomatitis (Fig. 2), tonsillitis of the lingual tonsil, paratonsillar and retropharyngeal abscess, Ludwig's angina (phlegmon of the floor of the mouth). With these diseases, drooling is possible, and inflammation of the paramygdaloid tissue and tissues of the floor of the mouth leads to trismus of the masticatory muscles (inability to open the mouth), a forced position of the head tilted to the painful side.
The occurrence of such a condition requires immediate contact with a medical specialist to sanitize the area of inflammation. Epiglottitis, an inflammation of the epiglottis caused by Haemophilus influenzae (more common in young children), gives similar symptoms. Along with refusal to eat, salivation, pain and hyperthermic symptoms, epiglottitis is accompanied by voice disturbance (it becomes dull, hoarse) and difficulty breathing. There is a forced position of the patient in a sniffing position, as if holding porridge in the mouth, the mouth opens freely, but a rough examination of the pharynx with a spatula can lead to laryngospasm and death. Therefore, with the above symptoms, pharyngoscopy is performed carefully; during it, you can see a hyperemic, edematous epiglottis behind the root of the tongue.
Other causes of sore throat accompanied by sore throat and cough can be in children and young people: drainage of discharge from the nasopharynx due to adenoiditis or sinusitis; irritation of the respiratory tract by dry air, smoke, including active and passive smoking; childhood infectious diseases [9]. In adults, a common cause of such complaints, often with a feeling of a lump in the throat, a “foreign body,” is an exacerbation of chronic pharyngitis associated with pathology of the gastrointestinal tract: gastritis, esophagitis, gastroesophageal reflux, cholecystitis, gastric ulcer. Severe dysphagia, regurgitation and pain when swallowing can be caused by esophageal varices [14].
A carefully collected anamnesis allows us to find out the dynamics of complaints, the time of their appearance, the connection with a previous injury or medical examination (gastroscopy), foreign body entry, contact with an infectious patient, hypothermia (drinking cold beer, ice cream), occupational or household hazards (irritants, dust , hot air, taking concentrated solutions of vinegar, spices, medications: corticosteroids, antibiotics, diuretics, local decongestants and others). Sore throat can occur as a manifestation of sexually transmitted diseases: gonococcal pharyngitis, syphilis, chlamydia of the respiratory tract. Infection with the human immunodeficiency virus contributes to the formation of inflammatory viral, tumor and mycotic lesions of the mucous membranes [3].
Chronic pathology of the kidneys, endocrine system, blood, previous radiation and chemotherapy can lead to the formation of a chronic inflammatory and atrophic process in the pharynx. The first manifestation of hyperglycemia [5] may be thirst and dry mouth, accompanied by catarrhal changes in the pharynx. Similar complaints occur with Itsenko–Cushing syndrome [5]. In patients with hypothyroidism, swallowing is often impaired, speech becomes slurred due to swelling and dryness of the tongue and lips, and it is difficult to perform pharyngoscopy.
Non-infectious pathology of the organs of the neck and chest cavity - angina pectoris, myocardial infarction - can manifest itself as intense pain in the pharynx and behind the sternum. Long-lasting dysphagia and unpleasant sensations in the form of a lump or foreign body in the throat, which are not amenable to anti-inflammatory therapy, can cause [14] tumors of the larynx, laryngopharynx, thyroid gland, and pharyngoesophageal (Zencker) diverticula. Many days of fasting, dieting, dyspepsia and heavy menstruation lead to a deficiency of vitamins and minerals. Vitamin A deficiency [5] causes dryness and erosion of the mucous membranes.
Vitamin B2 deficiency produces a triad of symptoms: dermatitis, cheilitis and glossitis (bright red, smooth and shiny dry tongue), accompanied by burning and pain in the mouth when talking and eating. Vitamin C hypovitaminosis occurs with dietary deficiency of ascorbic acid, inflammatory processes in the intestines and is manifested by pain, hemorrhagic and ulcerative-necrotic manifestations in the oral cavity and in the area of the palatine tonsils, mobility and tooth loss. Similar changes in the oral cavity and pharynx give rise to blood diseases (leukemia). Against the background of iron loss (with hyperpolymenorrhea), Plammer-Vinson syndrome is formed, characterized by superficial glossitis, dysphagia, cracks in the corners of the mouth, nail dystrophy, seborrheic dermatitis of the face, blepharitis, conjunctivitis, and decreased vision at dusk. B12 deficiency anemia associated with impaired absorption of this vitamin in the stomach due to anacid gastritis, tapeworm infestation, or increased consumption in pregnant women, manifested by Möller-Gunter glossitis (bright red tongue with smoothed papillae) and atrophy of the pharyngeal mucosa, burning pain in the tongue, weakness, crawling sensation in the limbs. A blood test reveals macrocytes, megalocytes, hyperchromic anemia, leukopenia.
Diseases of the spine [2] (cervical osteochondrosis, tuberculous spondylitis, radiculitis) can cause pain in the pharynx. Neuralgia of the glossopharyngeal nerve manifests itself as intense pain in the pharynx, especially against the background of chronic stress in anxious and suspicious patients. Metabolic disorders, intoxication, and trauma contribute to its occurrence. Characterized by unilateral pain in the root of the tongue, tonsil, lasting several minutes, accompanied by dry throat and subsequent hypersalivation. The therapeutic effect is achieved by lubricating the root of the tongue and pharynx with local anesthetics. Neuralgia of the superior laryngeal nerve [1, 6] gives similar symptoms, but also includes a painful dry cough and spasm of the vocal folds during inspiration [6].
Pain in the pharynx can be caused by an odontogenic process: periodontitis, teething pathology, galvanism [4, 17]. Rarely, unilateral pain in the pharynx occurs, the cause of which is the long styloid process (Eagle syndrome), accessible to palpation in the area of the palatine tonsil [15].
Rare causes of pain in the pharynx are ulcerations on the mucous membrane of tuberculous etiology [14]. In this case, there is a prolonged cough, weight loss, and swollen lymph nodes.
A final diagnosis is possible based on oropharyngoscopy. The main differential diagnosis for pain in the pharynx is between its most common causes - acute (or exacerbation of chronic) pharyngitis and sore throats caused by streptococcal infection (group A beta-hemolytic streptococcus - GABHS).
Acute pharyngitis is a viral infection of the pharynx in 90% of cases. Its main symptoms are: increased body temperature, sore throat when the throat is empty, when eating, soreness and a dry cough that does not bring relief. Patients indicate the localization of unpleasant sensations on the back wall of the pharynx. In the pharynx (Fig. 3), hyperemia of all parts is detected: the posterior wall, arches, tonsils, and there may be vesicular rashes (herpes, enterovirus). Plaques are not typical, there is often a runny nose and other catarrhal phenomena - nasal congestion, sneezing. If a rash is detected on the skin and mucous membranes, it is necessary to exclude an infectious disease - measles, scarlet fever, rubella [8]. Adenoviral infection manifests itself in the form of conjunctivitis, enlarged lymph nodes, fever, runny nose, and there may be plaque in the throat.
The disease progresses in waves: on the 7th–10th day of illness, a repeated increase in body temperature and a return of symptoms are possible. Enterovirus infection (“summer flu”) manifests itself in the form of dyspeptic, myalgic, and meningeal syndromes. Pharyngoscopy reveals bubbles on the mucous membrane of the oropharynx. In making the diagnosis of viral pharyngitis, the following help: knowledge of the epidemiological situation, dynamic observation of the patient, a variety of clinical manifestations (abdominal pain, vomiting, eye damage, meningeal symptoms, myalgia), lymphocytosis in the blood with normal ESR, lack of effect from antibacterial therapy, serological data research, polymerase chain reaction and others.
Sore throat is a general infectious disease with local manifestations in the form of acute inflammation of one or more components of the lymphadenoid pharyngeal ring, most often the palatine tonsils (tonsillitis), pharyngeal tonsil (adenoiditis), lingual tonsil, lateral ridges of the pharynx and larynx.
The classification of acute tonsillitis (according to I.B. Soldatov, 1975) involves the division into primary tonsillitis: catarrhal, lacunar, follicular, ulcerative-membranous; and secondary: for acute infectious diseases (diphtheria, scarlet fever, measles, tularemia, typhoid fever, infectious mononucleosis) and diseases of the blood system (agranulocytosis, alimentary-toxic aleukia, leukemia). There are special forms of tonsillitis [10]: viral, fungal, syphilitic.
With catarrhal tonsillitis, there is hyperemia and enlargement of the palatine tonsils, regional lymphadenitis, no plaque, a blood test shows slight leukocytosis, increased ESR. Catarrhal sore throat often has to be differentiated from viral pharyngitis, in which there is a cough, there may be a runny nose, and there is no enlargement or tenderness of the lymph nodes.
Follicular tonsillitis is manifested by bright hyperemia and swelling of the tonsils, subepithelial rounded yellowish elevations (follicles).
With lacunar tonsillitis, white-yellow plaques appear at the mouths of the lacunae of the tonsils (Fig. 4), which can merge with each other and cover the entire surface without going beyond the tonsils, being removed without leaving a bleeding surface, rubbing between two spatulas, dissolving in the vessel with water.
It is important to determine the streptococcal etiology of acute tonsillitis. This can be done using the McIsaac screening scale [12], which includes symptoms and their assessment in points (
).
A patient’s symptoms with a score of 3 means the probability of streptococcal etiology is 30%, and a score of 4 means about 70%. If the clinical picture is determined to be 0–1 points, then systemic antibiotic therapy is not indicated. At 2–3 points, antibiotics are necessary only if the infection is bacteriologically confirmed. Antibiotics should be prescribed when symptoms of 4–5 points are detected.
Diphtheria of the pharynx occurs in the form of localized, widespread, toxic I, II, III degrees and hypertoxic forms. With it, gray plaques are detected on the surface of the tonsils, tightly fused with the underlying tissues, they may spread to the arches, the mucous membrane of the posterior pharyngeal wall, the uvula (Fig. 5), and when you try to remove them, the mucous membrane bleeds. Plaques do not rub down and do not dissolve in water. In the toxic form, the neck is noticeably thickened due to swelling of the subcutaneous fat, pressure is painless and does not leave pits.
Infectious mononucleosis is an acute infectious disease caused by the Epstein-Barr virus, characterized by fever, sore throat, enlarged lymph nodes, pharyngeal tonsil, liver, and spleen. Plaques on the tonsils, as in lacunar tonsillitis (Fig. 6), but can spread beyond them. A general blood test (the appearance of atypical mononuclear cells), serological research methods (enzyme-linked immunosorbent assay (ELISA), Paul-Bunnel-Davidson reaction) help in diagnosing the disease.
Fungal infections of the pharynx in the form of curdled films, easily removed when scraped with a spatula, are caused mainly by yeast-like fungi of the genus Candida (about 90% of cases); less commonly, there are mold fungi of the genus Aspergillus, Penicillium [7]. C. albicans permanently or temporarily lives on human mucous membranes, skin and intestines. Factors contributing to the development of mycoses are: treatment with broad-spectrum antibacterial drugs, cytostatics and corticosteroids, diabetes mellitus, blood diseases, tumors, gastrointestinal diseases, vitamin imbalance. Candidiasis of the oral cavity, pharynx and esophagus occurs in more than 90% of AIDS patients (Fig. 7) [3].
Diagnosis of sore throats should include throat and nasal swabs for diphtheria (BL). Express determination of streptococcal antigen using test strips from the surface of the tonsils makes it possible to justify antibacterial therapy. A general blood test facilitates the differential diagnosis of primary and secondary acute tonsillitis. Opinions on the question “Should I do a smear?” controversial. It is needed to confirm the GABHS etiology of the disease in doubtful cases [16].
Therapeutic tactics for pain in the pharynx can be presented in the form of a diagram ().
For the treatment of acute pharyngitis, a gentle diet, hot foot baths, warm compresses on the front surface of the neck, warm alkaline drink (mineral water, milk with honey), steam inhalations, and smoking cessation are recommended. The attitude towards gargling is ambiguous [16]. Fresh infusions of mint, chamomile, calendula, eucalyptus, sage, and caragana are effective for relieving sore throat. Antiseptics of artificial origin (dichlorobenzene, metacresol, hexethidine, benzalkonium, thymol, ambazone, chlorhexidine) are bactericidal in their mechanism of action, which can lead to suppression of the normal microflora of the oral cavity, so they should be used with caution in children under 6 years of age [9]. For the treatment of sore throat, the most important painkillers are those containing menthol, tetracaine, lidocaine or flurbiprofen. Children from 6 months of age can use the herbal preparation Tonsilgon, which has an antiseptic and analgesic effect, but does not contain either menthol or lidocaine.
Menthol preparations and any sprays cannot be used before 3 years of age due to the possible development of laryngospasm.
Local combination drugs (antiseptics and painkillers) in the form of finished dosage forms are the most popular for the treatment of sore throat. One of them is TheraFlu LAR, a universal and highly effective local drug with an antiseptic and analgesic effect. TheraFlu LAR contains benzoxonium chloride and lidocaine. Available in the form of a spray and tablets, the content of lidocaine in which is 0–75 mg and 1 mg, respectively.
Recent in vitro and in vivo studies confirm the broad antiseptic spectrum of benzoxonium chloride and its activity against the main pathogens of the most common diseases of the oral cavity and pharynx. At the same time, the balance of the bacterial flora in the mouth is not disturbed, even with prolonged use of benzoxonium chloride.
Benzoxonium chloride has:
- bactericidal effect against aerobic and anaerobic gram-positive and gram-negative bacteria;
- fungicidal effect against Candida albicans, Aspergillus spp. and yeast fungi;
- antiviral activity against membrane viruses, including herpes virus, influenza virus, parainfluenza viruses, the causative agent of vesicular stomatitis.
Lidocaine is a local anesthetic that reduces pain in the throat when swallowing.
Adults should take the drug 1 lozenge every 2–3 hours (no more than 10 tablets per day) or as a spray, 4 sprays 3–6 times a day. Children aged 4 years and older are prescribed 1 lozenge every 2-3 hours (no more than 6 tablets per day) or as a spray, 2-3 sprays 3-6 times a day. The required duration of treatment, as a rule, does not exceed five days. The drug is well tolerated by patients, side effects are recorded extremely rarely. Possible short-term local irritation of the mucous membrane, allergic reactions.
Indications for its use are: pharyngitis, laryngitis, catarrhal tonsillitis, stomatitis, ulcerative gingivitis. Contraindications to the use of TheraFlu LAR: pregnancy (first trimester), breastfeeding, hypersensitivity to lidocaine, children under 4 years of age. TheraFlu LAR can be used by people with diabetes, as it does not contain sugar. Thanks to the combined effect - antibacterial and analgesic, TeraFlu LAR can relieve all symptoms of viral pharyngitis and be used in the complex therapy of bacterial sore throats.
Systemic antibiotic therapy in the treatment of patients with “sore throat” is indicated mainly for acute tonsillitis (angina) of suspected or established streptococcal etiology (GABHS) and is carried out with penicillins, and if they are intolerant, with macrolides; cefuroxime (Axetin) is effective. Clindamycin and lincomycin are reserve drugs [11]. Epiglottitis caused by Haemophilus influenzae is effectively treated with protected penicillins.
Literature
- Alimetov Kh. A. Secondary neuropathy of the upper laryngeal nerve / M materials of the anniversary All-Russian. scientific-practical conf. with international participation “Modern aspects and prospects for the development of otorhinolaryngology. M., September 29–30, 2005. P. 46.
- Alimetov Kh. A. Spondylogenic pharyngeal dyskinesia / Materials of the anniversary All-Russian. scientific-practical conf. with international participation “Modern aspects and prospects for the development of otorhinolaryngology. M., September 29–30, 2005. P. 22.
- Bessarab T.P., Yushchuk N.D., Anyutin R.G., Potekaev S.N. HIV infection in otorhinolaryngological practice // Attending Doctor, 2000. No. 1. P. 26–30.
- Inflammatory diseases of the mucous membrane of the pharynx, oral cavity and periodontium. Scientific review. Solvay pharma, 2002. P. 2.
- Diseases of the mucous membrane of the oral cavity and lips / Ed. E. V. Borovsky, A. L. Mashkilleyson. 1984. 400 p.
- Karpova O. Yu. Clinic, diagnosis and treatment of laryngoneurosis / Materials of the anniversary All-Russian. scientific-practical conf. with international participation “Modern aspects and prospects for the development of otorhinolaryngology. M., September 29–30, 2005. P. 53.
- Kunelskaya V. Ya., Kasimov K. On the issue of the clinic, diagnosis and treatment of candidal tonsillitis in children // Vestn. otorhinolaryngology. 1980. No. 4. P. 50–52.
- Nisevich N. I., Uchaikin V. F. Infectious diseases in children. M.: Medicine, 1985. 298 p.
- Acute respiratory diseases in children: treatment and prevention. Scientific and practical program of the Union of Pediatricians of Russia / Ed. A. A. Baranova. M., 2008.
- Otorhinolaryngology: national guide / Ed. V. T. Palchuna. M.: GEOTAR-Media, 2008. 960 p.
- Rational antimicrobial pharmacotherapy: Hand. for practicing doctors. Under general ed. V. P. Yakovleva, S. V. Yakovleva. M.: Litterra, 2003. 108 p.
- Sidorenko S.V., Guchev I.A. Tonsillopharyngitis: issues of diagnosis and antibacterial therapy // Consilium medicum. Infections and antimicrobial therapy. 2004. 4: 36–38.
- Folomeeva O. M., Amirdzhanova V. N., Yakusheva E. O. et al. Incidence of rheumatic diseases in the Russian population (analysis over 10 years) // Ter. Archive. 2002. No. 5. P. 5–11.
- Shevrygin B.V., Mchedlidze T.P. Handbook of otorhinolaryngology. M.: Triada-X, 1998. 448 p.
- Shulga I. A., Zaitsev N. V., Zaitseva V. S. Variants of the structure of the stylohyoid complex / Materials of the Anniversary All-Russian. scientific-practical conf. with international participation “Modern aspects and prospects for the development of otorhinolaryngology. M., September 29–30, 2005. P. 75.
- Etiopathogenetic therapy of diseases of the upper respiratory tract and ear: Methodological recommendations. Compiled by S.V. Ryazantsev, Kotserovets V.I. St. Petersburg: National Register, 2008. 100 p.
- Yakovleva V.I. Diagnosis and treatment of neurogenic diseases of the maxillofacial region: Textbook. manual for institutes and faculties. improved doctors. Minsk: Vysh. school, 1989. 102 p.
M. V. Subbotina , Candidate of Medical Sciences Irkutsk State Medical University , Irkutsk
Contact information about the author for correspondence
Symptoms of glossitis
- increased salivation;
- swelling and redness;
- pain and burning when eating;
- plaque on the tongue in the form of spots;
- bad breath;
- papillomas or warts on the tongue;
- speech disorder;
- foreign body sensation.
Prevention of glossitis - high-quality oral hygiene and no bad habits. It is important to undergo timely preventive examinations and also eat well. All these factors actively contribute to the development of the disease and bring a number of problems.
Inflammation of the lingual tonsil
A rather rare complication of tonsillitis, which manifests itself against a background of weakened immunity, is angioma - inflammation of the lingual tonsil, which is located at the root of the tongue. Despite its rarity, this disease is complex and painful, and lack of treatment threatens the patient not only with pain at the root of the tongue, but also with serious complications such as rheumatism, polyarthritis, sepsis and myocarditis.
The symptoms characteristic of angioma are similar to those of ordinary sore throat, but are noticeably more severe and have a number of specific differences:
- temperature increase;
- pain when swallowing;
- enlarged lymph nodes;
- swelling of the tongue;
- impaired immunity;
- probable appearance of purulent plaque.
Sore throat often causes pain in the root of the tongue.
The patient complains of severe pain in the deep parts of the throat, which also intensifies with active movements of the tongue (especially when moving it forward). Swelling causes difficulty breathing, swallowing and speech, and worsened inflammation leads to severe migraines.
Treatment of angioma depends on the degree of neglect of the disease, and in the early stages coincides with the principles of treatment of acute sore throat: taking vitamins, drinking warm liquids, inhalation, rinsing with soda solutions or decoctions. In more serious cases, ice is applied to the throat, alternating with warm compresses, and antibiotics and painkillers are also prescribed.
If the diagnosed symptoms include an abscess, the doctor may need to open it to relieve the patient's condition.
Treatment of glossitis
A specialist must make an accurate diagnosis and identify the cause of the disease. If you suspect that you have glossitis , and all symptoms indicate this, contact your dental clinic. This is the only way to create the right treatment plan and provide timely assistance. Quite often in such cases, doctors prescribe antibiotics, anti-inflammatory drugs and rinsing the mouth with special antiseptic solutions. In advanced stages, glossitis is treated surgically. Deep abscesses must be opened in the maxillofacial department. Under no circumstances should you take medications without a doctor’s recommendation.
You can cure glossitis, caries or any other diseases of the oral cavity right in your sleep. Family Dentistry Center "Medexpert" provides dental treatment under medicinal sedation. Thanks to this approach, the patient falls into a healthy sleep, ceases to feel pain and discomfort, while the vital functions of the body remain unchanged. Sedation is widely used in pediatric dentistry and even helps fight dental phobia. Dental treatment can be comfortable and painless - tested for yourself.
Diagnostics
To make a diagnosis, you should consult a dentist. If the cause is not of a dental nature, then you need to undergo an examination to identify the true causes of the disease. The following methods are used for diagnosis:
- collection . At the first visit, the patient outlines complaints, existing allergic reactions or injuries, chronic diseases, etc.
- Visual inspection. The doctor assesses the patient's condition based on the existing signs. If it is possible to eliminate the problem immediately, surgical manipulations are carried out. For example, removing a bone from the tongue.
- A clinical blood test to determine the presence of an inflammatory process in the body.
When a disease is detected, the doctor determines treatment tactics.
What to do?
Of course, says the ENT doctor, every person can look into his own throat with the help of an ordinary flashlight and mirror. However, you should not turn into your own doctor, warns Vladimir Zaitsev. “Because, for example, the use of antibiotics where it is not required, but antiseptics are needed, can seriously harm. For the same pharyngomycosis, the use of antibiotics will further suppress the flora and allow more active growth of fungi. It is also dangerous not to use antibiotics where they are required. And only a doctor can determine exactly what exactly, in what situation and what courses will be required,” says Vladimir Zaitsev. This means that if you experience a sore throat, an in-person examination and the prescription of adequate therapy are required.
There are contraindications. Be sure to consult your doctor.
Forms
Types of glossitis:
- deep;
- desquamative;
- diamond-shaped;
- villous;
- folded;
- Gunter's;
- syphilitic or interstitial.
The most dangerous is deep glossitis. The pathological process begins on the lower part of the tongue, and if left untreated, spreads to the floor of the oral cavity. In the case of abscess formation, the purulent process can spread to the neck, which is a life-threatening condition.
Desquamative glossitis is better known as “geographic tongue.” Irregularly shaped areas of peeling alternate with normal ones, so the tongue looks like a geographical map. This type of disease is typical for patients with chronic lesions of the digestive system, allergies, helminthic infestations, and can also occur during pregnancy.
Diamond-shaped lesions are typical for patients with chronic gastropathology. The disease is recurrent.
Villous glossitis occurs due to hypertrophy of the papillae of the tongue. This disease is one of the manifestations of a fungal infection - candidiasis, and can also occur in smokers.
The disease may be congenital. Such anomalies include a folded shape. This glossitis does not cause unpleasant symptoms and does not require special treatment.
Gunter's tongue is not an independent pathology, but one of the manifestations caused by anemia resulting from a lack of vitamin B 12 and folic acid in the body. The disease develops gradually. The mucous membrane of the tongue becomes smooth, the papillae decrease in size, and the tongue acquires a crimson hue.
Interstitial glossitis is also a secondary manifestation and is characteristic of patients with syphilis. The pathological process proceeds deeply, affecting muscle tissue. If left untreated, the muscles are replaced by connective tissue, which is an irreversible process. This form can transform into a malignant tumor.
Having seen photos of glossitis of different etiologies, you can be convinced that the clinical symptoms of this disease are varied, so only a specialist can make a differential diagnosis.
Glossitis of the tongue can be either an independent disease or one of the clinical symptoms of another pathology. For proper treatment, it is necessary to find out whether the disease is a primary inflammatory process, or arose as a result of changes in other organs and systems.
Swollen lips
As mentioned above, the tongue and lips most often swell at the same time due to allergies. In this case, swelling occurs rapidly, literally in a matter of minutes. Along with a swollen tongue, the patient may experience other unpleasant symptoms, such as a runny nose, sneezing, mild cough, vomiting and abdominal pain. If no measures are taken, then other symptoms may appear a little later - such as increased body temperature, changes in body color and sensitivity, and soreness and swelling of the tongue.
Many in this situation are lost and do not know what to do if the tongue is swollen and the patient apparently has an allergic reaction. You should not panic, you need to act quickly and clearly. You need to urgently call an ambulance, and before it arrives, give the patient an antihistamine, open the windows wide and provide access to fresh air, and avoid contact with the allergen (if known).