Stomatitis is a disease that can be caused by dozens of reasons, and often, even with the correct doctor’s prescriptions, both young patients and adults suffer from the inability to speak and eat normally for 5-7 days. And this is during the normal course of the disease. In severe cases, the disease does not subside for 2-3 weeks, and when asked how long stomatitis lasts, even the doctor shrugs.
- What determines the speed of recovery?
- How many days does it take for stomatitis to go away?
- How long does stomatitis last in children?
- How to understand that stomatitis has passed?
- Can stomatitis go away on its own?
- Consequences of advanced stomatitis
- Why can stomatitis not go away for a long time?
- What to do if stomatitis does not go away?
- How to prevent relapse?
The choice of a particular treatment method depends on the complexity of the problem and the stage of its development.
By clicking the “request a call” button, you agree to the personal data processing policy.
What determines the speed of recovery?
With timely consultation with a doctor and proper treatment, the acute form of stomatitis can be cured in 3-7 days.
Optimistic forecasts are not always justified: too many factors influence the duration of the disease. Among them:
- reasons that caused the disease. So, for careless handling of the fork you will have to pay with 2-3 days of discomfort. But allergic stomatitis will not go away until the doctor identifies the allergen;
- correct diagnosis . Treatment of viral stomatitis is fundamentally different from fungal stomatitis, and prescriptions for the catarrhal variety have nothing to do with the list of measures necessary to treat the nicotine form;
- treatment literacy . And here only the professionalism and experience of the doctor will help;
- accuracy of compliance with recommendations . An interrupted course of antibiotic therapy, ignoring the need for further examination by other specialists, omissions in taking medications - all this prolongs the course of the disease;
- state of immunity . The lower the body’s protective function, the higher the likelihood of developing stomatitis and the longer the recovery period.
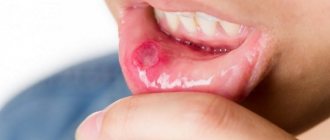
At the first symptoms: burning of the mucous membranes, unpleasant itching, the appearance of small but painful ulcers on the palate, inner surface of the lips or cheeks, you need to consult a dentist as soon as possible. After all, the main danger of stomatitis is its transition to an advanced form. And then treatment will take a long time and not always successfully. The risk factors here are:
- taking medications
that reduce immunity and disrupt intestinal microflora, for example, antibiotics; - vitamin deficiency
, including seasonal; - weakened immunity
. That is why it is absolutely impossible to let stomatitis take its course in infants, elderly people and pregnant women; - disruptions and restructuring of the hormonal system
. And again, expectant mothers are targeted, and along with them, teenagers in the transition period; - chronic diseases of the gastrointestinal tract, oral cavity, endocrine system
.
Even constant stress at work or misunderstandings in the family can cause stomatitis and its transition to a chronic form. Moreover, to completely cure the disease in this case, the efforts of the patient and the dentist are not enough. You will need to completely change your habits, diet, establish sleep and rest patterns, and even consult a psychologist.
Causes
Among the causes of stomatitis in adults, general and local ones are distinguished1. The latter include any damaging factors that act directly on the mucous membrane (too hot food, chemicals, mechanical damage), the general ones include chronic diseases of internal organs not related to the oral cavity (infectious, allergic, systemic), as well as metabolic disorders substances1.
In the first place in terms of prevalence are infectious stomatitis - viral, fungal or bacterial2.
The presence of various microorganisms in the oral cavity is normal. In a healthy, intact state, the mucous membrane can resist infection. However, with a decrease in local immunity, injury or poor hygiene, pathogens can penetrate deeper layers and cause inflammation1,3,4.
The soft tissues of the oral cavity can be injured by improperly fitted dentures, pieces of food or sharp chips on the teeth. Inflammation is often provoked by thermal or chemical factors, for example, very hot or spicy food, cosmetics3.
The following factors also contribute to the development of stomatitis3,4,6:
- allergic reactions1;
- poor oral hygiene;
- dental diseases;
- heredity;
- stress;
- hormonal disorders;
- diseases of the gastrointestinal tract;
- smoking.
A drug can become an irritant that provokes inflammation; for example, stomatitis in patients with bronchial asthma occurs during the use of inhalers with glucocorticosteroids (hormonal anti-inflammatory drugs)3. Also, the protective barrier of the mucous membrane is exposed to harmful substances in the air with which a person comes into contact due to professional activities3,5.
How many days does it take for stomatitis to go away?
Dentists, like doctors of other specialties, really don’t like asking patients about recovery time. But statistics on the cure of various forms of the disease still exist. And the patient has the right to know how quickly he will restore his health.
Aphthous (bacterial) stomatitis
Causes:
The causative agents of aphthous stomatitis are streptococci, staphylococci, gonococci, mycobacteria, Helicobacter pylori.
Features of the flow:
This form of stomatitis got its name from the name of superficial ulcers on the mucous membrane - aft. They are formed at the slightest decrease in immunity, for example, in spring or autumn, if an untreated bacterial infection is lurking in the patient’s body.
In addition to damage to the mucous membranes of the mouth, acute bacterial stomatitis causes fever and inflammation of the submandibular lymph nodes. The most unpleasant thing about the disease is its very rapid transition to a chronic form and constant relapses.
Treatment:
It is simple to classify aphthous stomatitis, as well as to cure its acute form. For this purpose, rinses with antiseptics (Chlorhexidine, Furacillin), antipyretics (Paracetamol), and antibiotics (Amoxicillin, Lincomycin) are prescribed.
To prevent the disease from becoming chronic, it is important to identify the pathogen. To do this, a bacterial culture of the afts is carried out, and blood tests may be prescribed for the presence of antibodies. And after determining the culprit of the disease, the dentist will hand over the patient to a specialized specialist: a therapist (pediatrician), gastroenterologist, infectious disease specialist or venereologist.
The recovery period with timely initiation of treatment for acute aphthous stomatitis is 7-10 days. When self-medicated, the disease quickly turns into an ulcerative form, which does not heal for months.
Viral stomatitis
Causes:
rarely - causative agents of measles, chickenpox, most often - causative agents of herpes. The infection is transmitted by contact and airborne droplets.
Features of the flow:
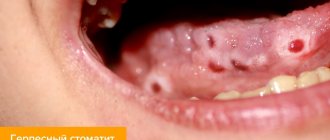
The disease is severe, with high fever, weakness, nausea and vomiting. Multiple small bubbles filled with liquid form on the mucous membrane. After 3-4 days they burst and heal. But with weakened immunity, new ones immediately form in their place.
Unfortunately, the herpes simplex virus instantly spreads both in the family and in children's groups. And most of us, without knowing it, are its carriers. While the immune system is in order, the virus quietly sleeps in the nerve ganglia. But if you get cold or nervous, stomatitis is right there.
Treatment:
at high temperatures, it is necessary to adhere to bed rest, take antiviral (Acyclovir, Gerpevir) and antipyretic drugs (Nurofen, Paracetamol). Treatment of the oral cavity with local antiseptics (Chlorhexidine) multiple times throughout the day is mandatory. To prevent infection of all household members, it is important to provide the patient with separate dishes and personal hygiene items.
The recovery time for viral stomatitis is 8-10 days. Local immunostimulants, for example, chewable tablets with echinacea, will help prevent the disease from becoming chronic.
Fungal stomatitis (candidiasis, thrush)
Causes:
The causative agent is the fungus Candida.
Features of the flow
: This form of stomatitis primarily affects children under 3 years of age. Adults are threatened with fungal stomatitis only in the case of a very strong decrease in immunity, for example, with long-term aggressive antibiotic therapy.
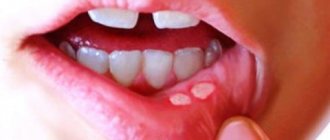
A characteristic feature of the disease is a white cheesy coating on the oral mucosa. At the initial stage, it is easy to remove with a regular napkin. Later, this process becomes painful, erosions and minor bleeding occur.
Treatment:
Since fungal stomatitis mainly affects children, doctors often prescribe decoctions of medicinal herbs, such as sage and chamomile, as antiseptics for treating the oral cavity. The treatment regimen must include antifungal drugs (Futsis, Fluconazole, Nystatin, Candida drops) and immunomodulators (Viferon, Interferon).
The recovery time for candidiasis directly depends on the state of the immune system. For some, therapy will help in 4-5 days, for others it will be difficult to overcome the disease in a month.
Catarrhal stomatitis
Causes:
poor oral hygiene, use of other people's personal hygiene items, pockets of infection in the mouth - caries, tartar, trauma to the mucous membrane from hot food, sharp objects, chipped teeth or fillings, biting the cheeks.
Features of the flow:
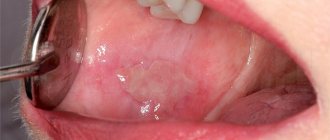
catarrhal stomatitis occurs more often than others. It does not give such vivid visual symptoms as aphthous or fungal, so it is often detected at a very advanced stage.
Often the only sign of catarrhal stomatitis for a long time is only bad breath. It cannot be removed by diet or careful hygiene. A little later, patients notice increased salivation and inflammation of the gums. After a while, a yellowish coating will appear on the tongue, and bleeding of the soft tissues will begin.
Treatment:
catarrhal stomatitis is perfectly curable. This does not require antibiotics or antifungals. It is enough to rinse your mouth several times a day with either a decoction of sage, chamomile, a solution of calendula tincture, or use the pharmaceutical antiseptic Chlorhexidine. The anti-inflammatory and analgesic drug Cholisal will also significantly speed up the healing process.
When the traumatic factor disappears, the exacerbation process does not last long: 3-5 days. But, if the cause is not eliminated, for example, a chipped tooth, the healing process will take longer each time. Over time, ulcerative necrotic lesions form on the mucous membrane, to combat which the dentist will have to use the entire arsenal of the most powerful medications.
Allergic stomatitis
Causes:
allergens, which can be food and medicine, oral care products, and even the materials from which fillings, crowns, and orthodontic systems are made.
Features of the flow:
allergic stomatitis is the most severe form of the disease. It begins with slight discomfort: swelling and redness of the mucous membrane. If contact with the allergen continues, erosions form on the gums, tongue, inner surface of the lips and cheeks, and unbearable itching appears.
Over time, it becomes painful for patients not only to talk and eat, but even to breathe air through their mouths. At the same time, the general condition is steadily deteriorating. And if the irritant is not removed, even Quincke's edema and death are possible. Fortunately, sluggish allergic stomatitis is much more common: it does not produce such pronounced symptoms and does not lead to death, although it torments the patient for years.
Treatment:
The main task of the doctor is to identify the causative agent of the allergy. Without this, no drugs will lead to recovery. You can temporarily stop an allergic reaction with antihistamines (Fenistil, Claritin).
The recovery time for allergic stomatitis directly depends on the speed of identifying the allergen and eliminating contact with it. Under the most favorable circumstances, the doctor will overcome the disease in 10-15 days.
Causes of stomatitis
Inflammation of the oral mucosa can be caused by various reasons.
- Mucosal injury6.
- Viral, bacterial or fungal infection6.
- Allergy2.
- Immunity disorders (autoallergy, that is, a reaction to one’s own altered tissues2).
- Diseases of the blood, digestive, cardiovascular, nervous and endocrine systems2.
- Hypovitaminosis - lack of vitamins C, B1, B12, E, D32.
- Common infectious processes: measles, rubella, scarlet fever and diphtheria, infectious mononucleosis, tuberculosis and others1.
Only a specialist can understand the causes of stomatitis. Therefore, if symptoms of the disease appear, you should definitely contact your dentist.
Inflammatory diseases of the oral cavity can occur in a child of any age6. Immaturity of the body is the primary factor predisposing to the occurrence of stomatitis in children under one year of age. The mucous membrane of the oral cavity during this period of a child’s life is very vulnerable, its natural protective properties are reduced. The immunity received from the mother during fetal development and which protected the baby immediately after birth weakens every day. Therefore, the infection easily penetrates the mucous membrane and causes its inflammation. Most often at this age, candidal stomatitis occurs, commonly called thrush1,6.
From the age of one to 3 years, children actively develop immune mechanisms to protect the oral mucosa (local immunity), but its permeability to viruses remains extremely high. Therefore, in a 2-3 year old child, stomatitis is more likely to be viral, in the vast majority of cases - herpetic1,3,4.
From 4 to 12 years of age, stomatitis in children is more often caused by allergic and autoimmune reactions. In particular, chronic aphthous forms of the disease occur during this period1.
Up to contents
How long does stomatitis last in children?
In children, just like in adults, the speed of recovery directly depends on the type of disease. Approximate period: 7-14 days. If you consult a doctor in a timely manner and start treatment immediately, this time is enough to cope with the disease.
Often recovery is delayed due to the fault of the parents themselves. For example, they did not monitor the timely taking of medications and the implementation of treatment procedures, ignored the doctor’s recommendation to take additional tests, or turned to a pediatric dentist only after long-term self-medication did not lead to a positive result.
But sometimes even the most responsible parents cannot cope with stomatitis for a long time. Alas, this happens. This disease is insidious and multifaceted, its course depends on many factors, and is often unpredictable even for an experienced doctor.
Candidal stomatitis
In 80% of healthy children, Candida fungi can be found in the oral cavity. They get there during childbirth, from nipples and pacifiers, from care products, in contact with the mother's skin, with food during eating and usually do not cause any problems. Candidal stomatitis, or thrush, occurs when immunity decreases1.
Predispose to the disease:
- prematurity and postmaturity;
- developmental defects and concomitant diseases;
- treatment with antibiotics and hormones;
- artificial feeding;
- poor care and poor feeding hygiene;
- Using the wrong nipples1.
What does candidal stomatitis look like? In children's mouths, whitish or whitish-gray dotted formations appear on the reddened mucous membrane. They merge into films of a cheesy nature; when the films are rejected, bright red painful erosions are formed. Because of the pain, the baby becomes restless, cries often, sleeps poorly, and refuses to eat1.
In severe cases of candidiasis, a cheesy coating may appear on the palate and on the lateral surfaces of the tongue, on the tonsils and the back wall of the pharynx - candidal tonsillitis and pharyngitis develop1.
If your child has a fungal infection, you should always consult a doctor; he will tell you how and what to treat the mucous membrane with candidal stomatitis, so that the child does not have complications and recovers faster. Treatment, as a rule, involves treating the oral cavity with drugs with antifungal activity (chlorhexidine, hexethidine). In severe cases of the disease, antifungal agents, probiotics and immunomodulators are prescribed1.
Up to contents
How to understand that stomatitis has passed?
The fact that the disease is a thing of the past is indicated by the complete return of dental health to the level that preceded the disease. This:
- disappearance of ulcers and aphthae;
- stop bleeding gums;
- extinction of the inflammatory process;
- no pain when talking or eating;
- getting rid of bad breath.
Despite the fact that recovery is obvious to the patient, only a doctor can put an end to treatment. As a rule, this does not require additional tests. Treatment regimens have been verified over years of experience, and a routine examination is quite sufficient to confirm a cure.
Often the patient’s well-being returns to normal after 2-3 days, the ulcers heal, and the pain recedes. It is important not to stop treatment at this point. Antibiotics, antiviral and antifungal drugs are taken in courses for a reason. Their duration directly depends on the life cycle of pathogens. To completely destroy some it will take 5 days, others – 20. And only a doctor can determine the duration of treatment!
If you ignore the prescriptions and stop taking the medications, stomatitis will return at the first slight decrease in immunity. And it will be more difficult to cure him.
Can stomatitis go away on its own?
Stomatitis can go away on its own without treatment, especially if we are talking about the catarrhal form. For example, while eating, the cheek was injured by a bone, and untreated caries caused infection of the wound. But the human immune system is in perfect order, and even if any infections are sleeping in the body, the defense system does not give them the slightest chance to wake up.
In this case, stomatitis will actually go away on its own in 5-7 days. But if you add at least rinses with antiseptics, recovery would occur within 3-4 days. But it’s not even the speed of healing that’s important, but the guarantees. So, if you consult a doctor in a timely manner, in 99% of cases the patient will be healthy within 2 weeks.
In the absence of treatment, the probability of forgetting about the problem in such a short period of time is less than 50%. For one simple reason: there are at least 5 varieties of the disease, and several times more pathogens. And only a doctor can determine the culprit of stomatitis.
If symptoms of stomatitis appear in a child, the parent’s task is to immediately seek professional help. For adults, we can recommend the following: if stomatitis does not go away on its own, there is no point in delaying visiting a doctor for longer than 7 days. Without medication, the disease will not go away.
Do not ignore preventive visits to the dentist.
It is enough to visit a specialist 1 – 2 times a year, which will allow you to promptly identify any dental problem at an early stage of development. This means that its elimination will be quick, easy and without complications.
By clicking the “request a call” button you agree to the personal data processing policy.
Viral stomatitis
About 80% of all stomatitis in children is caused by herpes viruses3,5. In approximately 70% of cases, the disease develops in children aged 1 to 3 years3,4.
The disease can occur in mild, moderate and severe forms.
With mild herpetic stomatitis, the general condition is practically not disturbed. Body temperature does not exceed 37-37.50 C. Symptoms of inflammation are limited to swelling of the gums and usually the simultaneous appearance of single painful herpetic blisters and erosions on the mucous membrane (no more than 6). After 1-2 days, the contours of the lesions are blurred, the rashes turn pale, and the erosions heal without scarring3.
With moderate stomatitis, the child’s temperature reaches 38-390 C and lasts until rashes continue to appear. General intoxication manifests itself in the form of weakness, headache, nausea. The child becomes capricious, lethargic, refuses to eat and play3.
As the temperature rises, the oral mucosa becomes red and swollen, and the gums begin to bleed. The number of herpetic elements reaches 20-25, repeated rashes are accompanied by fever3.
Severe stomatitis in children looks like a common acute infectious disease and is accompanied by severe intoxication: fever 39-400 C, chills, headache, aching muscles and joints, heart rhythm disturbances, nosebleeds, nausea and vomiting. The number of herpetic elements can reach 100; they are located not only in the mouth, but also on the skin of the face, on the eyelids and conjunctiva of the eyes, and earlobes. In addition, upper respiratory tract symptoms may be present.3
Treatment includes treating the affected area with painkillers and antiseptic drugs, antiviral therapy, drinking plenty of fluids, a balanced diet and proper nutrition3,5.
Up to contents
Consequences of advanced stomatitis
Complications of stomatitis are scary and varied. So, if treatment is not started in time for an infant, he will refuse to eat, which in turn will lead to weight loss and growth retardation. Lack of treatment for the disease at any age is guaranteed to reduce immunity, and is likely to provoke a sore throat or pharyngitis. Herpes stomatitis often results in decreased vision. And ignoring the aphthous form of the disease is fraught with scarring of soft tissues and even limiting the mobility of the jaw bones.
If bacterial stomatitis is left untreated, the disease very quickly turns into an intractable ulcerative form. If viral and fungal stomatitis is not treated, it will return again and again due to stress, colds, and vitamin deficiency. Well, the allergic form of the disease can even lead to death.
Symptoms of stomatitis
Light redness of the oral mucosa is the first symptom of stomatitis. Over time, they swell and a burning sensation appears. If treatment is not started at this stage, the redness is replaced by small oval or round ulcers, grayish or white, with a red halo and a film on top. Moreover, the tissue around them looks absolutely healthy. Mouth ulcers are very painful and make eating difficult. They appear on the inner surface of the cheeks and lips, under the tongue. In most cases, mild stomatitis manifests itself as one ulcer.
The appearance of several ulcers of larger size and depth, which sometimes merge into one, are signs of more severe forms of stomatitis. The appearance of ulcers is accompanied by fever, inflammation of the lymph nodes, general deterioration of health, headache, loss of appetite and constipation. Acute stomatitis is accompanied by severe pain in the mouth, which interferes with eating and speaking. In addition, there may be excessive salivation, a coating on the tongue, a bright red mouth, irritability, and vomiting after eating.
Why can stomatitis not go away for a long time?
If stomatitis is difficult to treat, most likely the disease has already become chronic or recurrent. The reason for this, with proper prescriptions and compliance with all doctor’s recommendations, may be:
- immunodeficiency states;
- chronic diseases of the nasopharynx: sinusitis, pharyngitis, tonsillitis;
- chronic diseases of the gastrointestinal tract: dysbacteriosis, colitis, gastritis, gastric ulcer;
- permanent injury to the gums and tongue from dental plaque, dentures, the edge of a chipped tooth or poorly fitting braces;
- allergies to toothpaste, mouthwash, medications, filling material.
Constant stress and depression have a detrimental effect on your health. They seriously reduce immunity, provoking the development of many diseases, including stomatitis.
Bad habits, such as smoking and eating seeds, also interfere with recovery. In both cases, the mucous membrane and tongue are constantly injured by hot smoke or the sharp edge of sunflower seeds.
Traumatic stomatitis
Inflammation of the mucous membrane in the mouth can be preceded by trauma: mechanical, thermal, chemical, radiation1,6.
Small children who put everything in their mouths can injure the mucous membranes with the sharp edges of toys or household items. Injuries often occur due to inept use of cutlery as a result of falls. In older children, stomatitis may be associated with a thermal burn, blows to the teeth, or the bad habit of chewing a pencil or pen. Sometimes the cause of inflammation is dental diseases and their treatment: sharp edges of damaged teeth and fillings, braces and aligners1.
When stomatitis develops in a child on the gum, on the inner surface of the cheek or in another place, the mucous membrane becomes red and swollen, and a painful erosion or ulcer may appear in the area of damage. Since there are many microorganisms in the mouth, there is always a risk of a bacterial or fungal infection1.
If the mucous membrane is constantly injured, painless whitish or whitish-gray layers may form on it.
In children under 1 year of age, stomatitis can be the result of using the wrong nipples: long, tight, irregularly shaped. The resulting Bednar aphthae are located in the area of the transition of the soft palate to the hard palate and are round erosions or ulcers1.
Treatment of traumatic stomatitis in children includes:
- elimination of traumatic factors;
- rinsing the mouth, irrigating the mucous membranes and treating wounds with drugs with an analgesic and antiseptic effect1.
Up to contents
What to do if stomatitis does not go away?
When the disease does not subside, the main thing is to be patient. If additional tests have not been done yet, now is the time to do them. If the dentist recommends seeing a gastroenterologist or otolaryngologist, you need to listen to him. He doesn't do this because he wants to get rid of the patient. It’s just that in some cases it is more effective to fight the disease not alone, but with a team of specialists. The main thing is to identify the cause of the disease. And, unfortunately, in rare cases this can take months.
Literature
- Khomenko L. A. Therapeutic dentistry of children. Textbook for university / ed. 2007 – pp. 643-722.
- Ismailova G. T. Chronic recurrent aphthous stomatitis // Bulletin of surgery of Kazakhstan. - 2011. - No. 4. — P. 124-125.
- Drobotko L.N., Strakhova S.Yu. Acute stomatitis in children // Issues of modern pediatrics. - 2010. - T. 9. - No. 2. - P. 146-149.
- Suerkulov E. S., Yuldashev I. M., Mamyraliev A. B., Toktosunova S. A., Tsepeleva A. S., Sooronbaev A. A. Prevalence and structure of the incidence of stomatitis in children // Bulletin of Science and Practice. 2022. T. 4. No. 11. — P. 91-96.
- Suerkulov E. S., Yuldashev I. M., Mamyraliev A. B., Zhumashova N. K., Yuldasheva G. I. Complex therapy of inflammatory diseases of the oral mucosa in children // Bulletin of Science and Practice. 2022. T. 5. No. 5. — P. 96-104.
- Pankrusheva T.A., Maravina I.N., Chekmareva M.S. Research on the development of the composition and technology of tablets for the treatment of stomatitis // Scientific result. Medicine and pharmacy. – T.4, No. 1, 2022. – P. 78-87.
- Instructions for medical use of the drug HEXORAL® aerosol: , .
- Instructions for medical use of the drug HEXORAL® solution: , .
- Instructions for medical use of the drug HEXORAL® TABS: , .
- Instructions for medical use of the drug HEXORAL® TABS CLASSIC: , .
- Instructions for medical use of the drug HEXORAL® TABS EXTRA: , .
Up to contents
How to prevent relapse?
If once stomatitis has already made itself felt, it is worth making some changes in your life that will help avoid relapse:
- do not put off dental treatment until later;
- do not ignore nasopharyngeal diseases;
- treat gastrointestinal problems in a timely manner;
- supplement your oral hygiene with a rinse and irrigator;
- Make a habit of eating vegetables or fruits at every meal;
- take a course of multivitamins twice a year;
- avoid injuring the oral mucosa with hot and cold foods;
- take care not only of your physical, but also of your mental health: get enough sleep, rest on time, pamper yourself.
It is especially important if you are prone to stomatitis to choose a competent dentist. At the first visit, you need to tell him about past problems so that the doctor can prevent the development of the disease. For example, be as careful as possible when removing tartar or immediately prescribe gum treatment with Metrogil Denta gel when installing a prosthesis.
The information is for reference only. Before treatment, consultation with a doctor is necessary.
How is stomatitis treated in adults?
Complex treatment should be carried out only under the supervision of a doctor. On the one hand, it is important to eliminate the cause of the disease, on the other hand, to alleviate the symptoms and stimulate the restoration of the oral mucosa. The doctor prescribes both local and general therapy, depending on the form of stomatitis.
The following groups of drugs may be used in treatment5:
- antibacterial, antiviral or antifungal (depending on the pathogen);
- antiallergic drugs;
- anti-inflammatory drugs;
- enzymes;
- agents that stimulate the restoration of the oral mucosa;
- drugs that enhance immunity and improve metabolism.
For some forms of stomatitis, the doctor may prescribe combination medications. For example, Metrogyl Denta®, which is indicated for the treatment of aphthous stomatitis7,8,10.
Metrogyl Denta® is a dental gel that contains metronidazole, which has an antibacterial effect, and the antiseptic chlorhexidine8. This combination can suppress the activity of various types of microorganisms and helps fight infection7,8.
Metrogyl Denta® is widely used in dentistry; it is approved by the Dental Association of Russia (StAR)9. The duration of treatment, dose and frequency of use is determined by the doctor, depending on the degree of damage and severity of the disease.
The appearance of stomatitis may mean that a person has a weakened immune system or that the mucous membrane has been affected by some damaging factor. And sometimes redness and painful sores in the mouth are symptoms of a chronic disease1. A dentist helps to understand the causes and cope with inflammation, and if stomatitis has “deeper roots,” specialized specialists are involved in the treatment. After therapy, it is important to do everything to prevent the disease from occurring again. You need to regularly visit the dentist, replace dentures if they cause mechanical injury, monitor oral hygiene and give up bad habits1,5.
The information in this article is for reference only and does not replace professional advice from a doctor. To make a diagnosis and prescribe treatment, consult a qualified specialist.
to come back to the beginning