WHAT IS PERIODONTAL
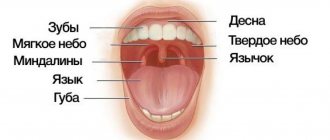
The periodontium is the complex of tissues surrounding the tooth. These include not only the gums, but also the bone socket in which the tooth root is located, and the tooth ligaments that hold the tooth in the socket, intertwined with the tooth root and bone. All these tissues represent a single system that performs several important functions at once: fixation of teeth, perception and regulation of chewing load, control of the work of masticatory muscles, protection against penetration of pathogenic bacteria and a number of damaging factors into the bone tissue.
HOW DOES GINGIVIT MANIFEST, AND WHY DOES IT OCCUR?
With superficial inflammation of the gums (if only soft gum tissue is involved in the process), we are dealing with gingivitis. Inflammation can occur in the area of 1 - 2 teeth (local gingivitis) or all teeth (generalized gingivitis).
Inflammation of the gums usually begins with damage to the gums, for example, when eating, brushing teeth, an incorrectly applied filling or crown, or a chemical burn. In this case, pathogenic microorganisms penetrate the injured gum and intensify the inflammatory response. The presence of soft plaque, tartar, and poor oral hygiene are mandatory conditions, and very often an independent cause of the onset and maintenance of the disease.
Gingivitis is often observed in people with malocclusions, crowded teeth and their incorrect position. A short frenulum of the upper and lower lips is also a risk factor for periodontal disease.
Smoking plays an important role (spasm of blood vessels occurs, gum nutrition deteriorates), decreased body defenses (immunodeficiency), lack of vitamin C and other risk factors.
In the acute stage of the process, pain, burning, swelling of the gingival margin, and bleeding when brushing teeth are usually noted. If the cause of the disease is not eliminated, then acute gingivitis becomes chronic, which does not go away on its own without treatment. In this case, the gums turn blue and periodically bleed when brushing your teeth and eating. There is an unpleasant odor from the mouth.
Severe forms of gingivitis, such as ulcerative gingivitis, are observed in severe general diseases of the body. For example, with diabetes or a serious immunodeficiency disease. In this case, the temperature rises, painful ulcers covered with a film appear on the dirty gray gums, and general health worsens.
With gingivitis, the teeth remain stable, since the process does not penetrate deep into the periodontium, the so-called periodontal pocket does not form, and the bone tissue of the tooth socket does not dissolve. Can there be consequences if gingivitis is not treated?
If gums are not treated in time, gingivitis will develop into periodontitis. This is a much more serious and dangerous disease than gingivitis. Often it becomes irreversible, since periodontitis affects and destroys the deep tissues of the periodontium - the ligaments of the tooth and the bone tissue of the jaw.
Classification of diseases of the oral mucosa
Stomatitis
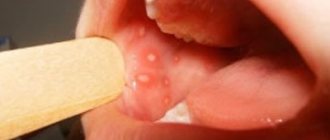
Stomatitis is an inflammation of the mucous membrane, characteristic of children and adults. Most often, stomatitis is bacterial, viral or fungal in nature. A bad toothbrush with hard, scratchy bristles, poorly fitting braces or crowns, and biting the cheeks and lips can also cause canker sores.
Most often, stomatitis manifests itself in the form of itchy, bright red or whitish sores and erosions on the inner surface of the cheek, tongue or gums. A person may complain of burning and swelling, bad breath, pain when chewing and swallowing. In advanced cases, the temperature may rise, sleep may be disturbed, and the person becomes irritable.
Glossitis
Glossitis is an inflammation of the tongue that can occur either as a result of injury (such as a burn), exposure to pathogens, or as a symptom of certain systemic diseases. Most often, glossitis is manifested by a burning sensation and discomfort in the mouth. The tongue becomes bright red and slightly swollen, and salivation may increase. The patient may complain of loss of taste or changes in the sense of taste, and eating or even just talking causes pain.
Highlit
Haylit (or cheilosis) is a disease in which the lips begin to peel, break, and “sticks” appear in the corners of the mouth. The reasons can be very different: exposure to wind and sun, allergic reaction, chronic diseases with skin lesions (dermatitis, psoriasis, etc.), endocrine pathologies or mycoses.
Oral leukoplakia
Oral leukoplakia is keratinization of the mucous membrane under the influence of aggressive factors, such as smoking. This condition is considered precancerous and therefore requires mandatory treatment.
Most often, oral leukoplakia appears as whitish, grayish, or red plaques that cannot be removed, rough or keratinized areas, or strange thickenings on the lining of the mouth. As a rule, the patient does not experience pain or discomfort, and therefore does not immediately consult a doctor.
Paradontosis
The periodontium is the complex of tissues that surround the tooth and hold it in place: the gums, periodontal ligament, periodontium, root cementum and bone tissue. Periodontal diseases include: gingivitis, periodontitis and periodontal disease.
Gingivitis
Gingivitis is an inflammation of the gums that most often occurs due to inadequate or irregular oral hygiene. Pathogens accumulate in plaque and tartar, causing inflammation.
With gingivitis, inflammation affects only the surface of the gums and may cause bleeding, swelling of the gums, mild pain or discomfort when pressing, and bad breath. If treatment is not started, the inflammation will go further and affect the periodontium.
Periodontitis and periodontal disease
Very often, patients confuse periodontitis and periodontal disease. Periodontitis is an inflammatory disease of periodontal tissues that causes bleeding gums and leads to the gradual exposure of tooth roots, their mobility and, as a result, their loss. Periodontal disease is a non-inflammatory periodontal disease in which the lining of the gums and jaw bone gradually decrease. Unlike periodontitis, in which tooth tissue is destroyed over several years, periodontal disease progresses very slowly and develops over decades. The patient may not even realize that he has gum disease. Periodontal disease is rare compared to other oral diseases.
WHAT FACTORS PROMOTE THE DEVELOPMENT OF PERIODONTITIS?
The causes of periodontitis are the same as those of gingivitis. Often periodontitis is associated with chronic gingivitis. If the traumatic factor persists, microorganisms actively continue to multiply in the damaged gum. Their toxins and enzymes destroy the gums deeper and deeper.
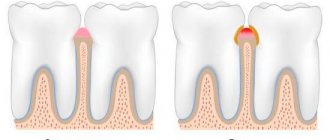
As a result, the connection between the gum and the tooth (the bottom of the periodontal sulcus) is disrupted - a very important protective formation that protects the tooth ligaments and bone from infection. A periodontal pocket appears, and now bacteria, plaque, etc. rush into the depths of the periodontium - this is where periodontitis begins. Next, gradual destruction of the tooth ligaments occurs, and the bone tissue melts.
Periodontitis can be acute or chronic. Typically, acute periodontitis occurs when there is deep, strong trauma to the gums (for example, a long artificial crown, a toothpick). In this case, the periodontal connection may be immediately disrupted - gingivitis and periodontitis occur simultaneously.
Generalized periodontitis is characteristic of serious general diseases of the body - diabetes, other endocrine diseases, radiation sickness, severe diseases of the gastrointestinal tract and cardiovascular system. It is almost impossible to cure such periodontitis without general treatment of the underlying disease.
In the chronic process, pain and swelling are not as pronounced as in acute periodontitis, the amount of tartar and soft plaque increases, the bad breath increases, the gums begin to settle, exposing the neck of the tooth, teeth become sensitive to cold, hot, sour and salty. Tooth mobility appears, unnoticeable at first, but steadily increasing.
Suppuration of periodontal pockets is often observed. Pus is released from under the gum when pressing on the gum edge with a finger. Sometimes, in the absence of outflow of pus, periodontal microabscesses occur - in this case, the patient already requires surgery.
Periodontitis can be one of the causes of some common diseases. The microorganism that causes stomach ulcers is often found in dental plaque. Other bacteria living in dental plaque can lead to the formation of microthrombi (blood clots). Penetrating into the blood (with bleeding gums), they increase the risk of cardiovascular diseases, including myocardial infarction. The entry of microorganisms into the blood can lead to septic endocarditis. There is information about the relationship between chronic dental and periodontal diseases and kidney damage. Remember that the focus of chronic infection in the oral cavity is the entry point for pathogenic bacteria into the body.
DIFFERENCES PERIODONTOSIS FROM PERIODONTITIS
Periodontal disease is a degenerative lesion of all periodontal tissues; this process never occurs in an acute form and is not associated with exposure to bacteria. There is a slow, uniform resorption of the bone tissue of the teeth cells and subsidence of the gums with exposure of the roots of the teeth. Periodontal disease is always a generalized process, that is, all teeth on both jaws are affected. Bone tissue atrophy is usually painless, continuous and, if left untreated, leads to the complete disappearance of the ligamentous apparatus, the walls of the tooth sockets and their loss. Inflammatory phenomena are associated with periodontal disease quite rarely.
The exact cause of the disease is still unknown. It is believed that the onset of the disease is associated with impaired blood circulation in periodontal tissues and endocrine disorders. The development of periodontal disease is promoted by diabetes, cirrhosis of the liver, gastric ulcer, neurogenic diseases, cardiovascular pathology (atherosclerosis), hypovitaminosis and a decrease in the body's overall resistance.
Local factors, for example, the impact of microorganisms on the periodontium, can only aggravate the course of the disease, therefore, in periodontal disease, the primary process is the resorption of bone tissue and the ligamentous apparatus of the tooth, and superficial changes in the gums are secondary.
Periodontal disease progresses slowly. Clinically, it manifests itself with significant changes in the periodontium. This is subsidence of the gums, exposure and increased sensitivity of the necks of the teeth, itching in the gums. Teeth remain stable for quite a long time.
A characteristic sign of periodontal disease is the presence of so-called wedge-shaped tooth defects - damage to the enamel of the teeth near the gums in the form of fairly deep oval cavities. Currently, this phenomenon is explained by a malnutrition of the tooth, inferior enamel and dentin, combined with very strong pressure on the toothbrush during frequent brushing. Periodontal disease is characterized by the absence of periodontal pockets.
WHY IS PLAQUE A MAIN CAUSE OF PERIODONTAL DISEASE?
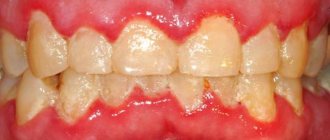
Bacterial plaque is a sticky, colorless film that constantly forms on teeth. If plaque is not removed, it will harden and form a rough, porous growth called tartar. Bacteria in tartar produce toxins (poisons) that irritate the gums, causing them to become red, tender, swollen, and bleeding. As the disease progresses, toxins can lead to periodontal destruction and the formation of pockets that fill with plaque. The bone that supports the teeth is subject to constant destruction. Consistently removing plaque through brushing, flossing, and professional care can minimize the risk of gum disease. However, if no treatment is given, the affected teeth may become loose and eventually fall out.
Gingivitis
An inflammatory process that causes swelling and tenderness of the soft tissues. If not treated in a timely manner, the problem worsens and becomes chronic.
The main causes of gingivitis:
- insufficient oral hygiene;
- thermal or chemical burns;
- use of certain medications;
- unbalanced diet (insufficient amount of vitamins in food)
- smoking;
- some infectious diseases;
- gastritis;
- ulcerative processes in the digestive system;
- caries.
Forms and types of gingivitis
Depending on the clinical situation and the nature of the development of the disease, acute and chronic gingivitis are distinguished. Acute gingivitis
manifests itself in the form of classic signs of the disease: redness, swelling and bleeding of the gums.
Chronic gingivitis
develops more quietly, without pronounced signs, but gradually leads to the growth of gum tissue (hyperplasia), which entails partial and complete coverage of the surface of the tooth crown by the gum.
Prevention measures
By following simple rules you can reduce the likelihood of serious oral diseases:
- Brushing your teeth at least 2 times a day after eating;
- Using dental floss and mouthwash;
- Balanced diet;
- Rejection of bad habits;
- Visit the dentist at least once every six months.
WHAT IS A PERIODONTAL EXAMINATION?
The history of the disease (anamnesis) is carefully determined. When did it first start, what was done for treatment, do parents and close relatives have this disease, etc. Careful collection of data makes it possible to determine risk factors and sometimes even predict the course of the disease. This is followed by a careful examination of the oral cavity: the frenulum of the lips and tongue, the dental arches as a whole and, if necessary, each tooth separately, as well as fillings, crowns and orthodontic appliances are assessed.
One of the main examination methods is probing the periodontal pocket of each tooth at six points. The presence of tartar and soft plaque, bleeding, suppuration, tooth mobility, etc. is assessed. This labor-intensive analysis is painlessly performed in 15 - 20 minutes using a special electronic probe of the automated computer clinical diagnostic system Florida Probe (USA). The patient’s personal data is stored in the computer’s memory, which makes it possible to predict the course of the process and select treatment, as well as evaluate the dynamics of the disease and the effectiveness of the treatment.
An orthopantomogram is a necessary element in the diagnosis of periodontal diseases. This image shows the teeth, jaw bones, and the partitions between the teeth. Digital orthopantomographs (such as the ones in our clinic) allow you to obtain excellent images with minimal radiation exposure to the patient and evaluate them on a computer screen using auxiliary computer programs.
Principles of treatment of diseases of the oral mucosa
Basic principles of treatment of diseases of the mucous membranes of the mouth, lips and tongue:
- Rational treatment requires contact between the dentist and other dental and non-dental professionals.
- Treatment must be carried out in compliance with the principles of bioethics, these diseases must be considered from the point of view of the state of the whole organism, therefore in most cases one cannot limit oneself to local effects only.
- An axiom for the dentist should be the elimination of all unfavorable irritating factors in the patient’s oral cavity that can support and provoke the development of the pathological process. The use of so-called cauterizing agents and prolonged use of the same mouth rinses is unacceptable.
- Treatment should begin only after at least one preliminary diagnosis has been established and the following requirements have been met: be comprehensive; provide a pathogenetic approach; do not violate the anatomical and physiological characteristics of the oral mucosa; eliminate the pain factor; promote rapid epithelization of lesions; provide for the active involvement of the patient in performing treatment procedures at home.
WHAT IS MEAN BY PERIODONTAL TREATMENT
After collecting all the necessary information, the periodontist will discuss the condition of your gums with you and suggest the most optimal treatment. Most importantly, it must be comprehensive - that is, treatment must cover all identified causes and associated factors that support the disease. Only in this case can it be possible to completely cure or stabilize periodontal disease for a long time.
Treatment will be much more effective if the patient strictly follows all instructions and strictly follows the chosen treatment plan.
Typically, a comprehensive treatment plan consists of general and local treatment and includes all or part of the methods listed below.
ELIMINATING TRAUMATORY FACTORS DURING TREATMENT
Treatment begins with the elimination of traumatic factors - low-quality fillings and crowns with an overhanging or very deeply embedded edge in the gum, bridges, traumatic teeth, etc. are removed.
The so-called selective grinding of teeth is carried out in order to eliminate excessive traumatic load when chewing from overloaded teeth. At the same time, small areas of the teeth are slightly undermined, which do not allow the upper and lower rows of teeth to meet correctly, thereby causing them to be overloaded.
This is an absolutely harmless procedure, since the ground areas of the teeth are polished and coated with fluoride preparations. In this case, caries does not occur.
Professional oral hygiene The next stage of treatment (performed in 100% of cases) is professional teeth cleaning: it allows you to remove even tartar located deep under the gum (this is the strongest traumatic factor). In addition to tartar and soft plaque, dense dark plaque (from smoking, drinking tea, coffee, and other dyes) is simultaneously removed - this allows you to restore the beautiful appearance of your teeth. After removing tartar and plaque, the doctor will definitely polish the cleaned surface of the root and crown of the tooth.
Nowadays, several methods of removing dental plaque are common. Cleaning teeth with a stream of air mixed with cleansing powder and water (the most famous representative is the Air Flow system) perfectly cleanses teeth of soft plaque, dark plaque from tobacco or coffee, even in hard-to-reach places. Ultrasonic scalers are capable of removing tartar of almost any size.
Removing tartar is one of the most important and effective stages in the treatment of periodontal diseases.
Anti-inflammatory therapy Drug therapy of gums allows you to relieve inflammation - cope with pain, swelling, and reduce bleeding gums. Typically, periodontal pockets are washed with antiseptic solutions (chlorhexidine, iodinol, etc.), and various medicinal substances are used (enzymes, antimicrobial, hormonal, anti-inflammatory drugs). Often the gums are covered with a special bandage after the medication is administered.
Self-absorbing Diplen-Dent films impregnated with various medications (antibacterial, improving blood circulation, etc.) are very convenient. Such films are glued by the patient independently to the affected areas of the gums (for example, before going to bed) and, gradually dissolving, release the medicine directly into the gums. In the morning, all you have to do is remove the remaining film from the oral cavity.
Physiotherapeutic treatment There are many methods of physiotherapeutic treatment of periodontal diseases. Laser therapy is most widely used in our clinic. Therapeutic laser radiation has a very wide range of therapeutic effects - relieves pain, improves blood circulation, metabolism, stimulates immune defense.
Gum massage can be performed by a doctor or independently. At home, use your index finger to massage the area of the interdental papilla of the gum with up and down movements (6 to 10 movements per papilla). The massage ends with hygienic rinses. Massage should not be used if the disease is exacerbating or if there are erosions or ulcers on the gums.
Surgical treatment Periodontal surgery is a radical and one of the most effective methods of treating moderate and severe periodontitis. With the help of small operations, it is possible to eliminate periodontal pockets, remove overgrown infected soft tissues, eliminate suppuration of the gums (microabscesses), replant bone tissue or bone substitutes, lift receding gums and close small root exposures.
Every year new developments in the field of surgical treatment, modern materials and treatment methods appear. One of the promising innovations is surgical treatment using cellular technologies, which allows stimulating the restoration of bone tissue. This technology is widely used in our clinic. Surgical treatment is always carried out after removal of dental plaque and therapeutic treatment, when all acute symptoms of gum inflammation subside. All interventions are performed under local anesthesia and rarely take much time. Usually all postoperative phenomena subside after 2 - 3 days, and the sutures are removed, or they dissolve within a week.
The effect of such operations often lasts for a long time. A lot will depend on maintaining oral hygiene, following preventative rules and overall health.
Rational prosthetics and splinting Prosthetics of missing teeth and their permanent splinting (i.e. joining teeth together using a prosthesis or special light-curing threads) are the final stage of the treatment of periodontal diseases. It allows you to fully restore the function of chewing, eliminate aesthetic defects (in the absence of teeth visible when smiling), and unite all the teeth together, as intended by nature.
In this case, the load is distributed evenly throughout the entire dentition, which allows the supporting teeth to function much longer. Even the absence of one tooth causes a number of changes in the bone tissue of the jaw. If, after successful therapeutic and surgical treatment of the gums, rational prosthetics and splinting are not carried out, then the disease may worsen again in the very near future.
Prosthetics are carried out using both removable and fixed dentures, depending on the condition and number of teeth.
After completion of treatment, we advise you to strictly follow all the doctor’s recommendations. Be sure to visit your doctor at least 1-2 times a year for a follow-up examination and professional oral hygiene.
Periodontitis
Periodontitis is an inflammation of periodontal tissues, which includes the teeth, ligaments, cementum and gums. Periodontitis as a disease is a consequence of gingivitis - a minor inflammation of the gums, the main cause of which is neglect of oral hygiene. If with gingivitis the inflammation spreads exclusively to the soft mucous membranes, then with periodontitis the ligaments that hold the teeth in the sockets are affected. This is why in 90% of cases when this disease is diagnosed, tooth mobility is observed, which eventually leads to their loss.
The most common causes of the disease are the following:
1. Improper or irregular oral care
. Dental plaque, which is present on the surface of the teeth and in the spaces between teeth, is not as safe a substance as it might seem at first glance. Soft and easily removed at the beginning, it goes through certain cycles of “development”. The result is the mineralization of plaque and its transformation into hard tartar. This process in most cases is observed in those who do not pay due attention to daily oral care or use an incorrectly selected toothbrush, toothpaste and mouthwash.
2. Poor blood supply to the gums
. Periodontitis is one of the most common problems among smokers. Substances contained in tobacco smoke lead to a narrowing of the blood vessels in the oral mucosa and their fragility, which impairs the blood supply to the gum tissue and supporting apparatus of the teeth. A slowdown in blood circulation and, as a consequence, the development of periodontitis is also facilitated by a lack of chewing load caused by eating habits (for example, the predominance of soft foods in the diet).
3. Nutrient Deficiency
. The lack of fresh vegetables, fruits, herbs, a sufficient amount of fish, meat and dairy products in the diet quickly leads to a lack of essential substances in the gum tissue. If poor nutrition is a permanent habit, then over time the metabolic processes in the gums are disrupted, which creates the ground for inflammation and periodontitis. A deficiency of vitamins A, C and group B can lead to negative consequences.
Treatment of periodontitis
Professional teeth cleaning is an integral step in the treatment of periodontitis. This procedure removes physical obstacles (plaque and tartar) that prevent the gums from returning to their previous position and tightly covering the teeth.
Drug treatment - the use of antiseptics for topical use. This need is due to the high risk of spread of inflammation and infection to other tissues.
Surgery
At an advanced stage of periodontitis, when the inflammation has spread deep into the bone tissue, surgical intervention becomes necessary. Such manipulations include partial excision of the gums (gingivectomy), washing of periodontal pockets with medicinal solutions, removal of stones, and flap operations. In some cases, surgical treatment of periodontitis involves the implantation of bone tissue substitutes or the application of collagen or artificial membranes to restore the supporting apparatus of the tooth.
Compliance with oral care rules
Without regularly removing plaque and protecting the oral cavity from bacteria, it is impossible to achieve sustainable results in the treatment of periodontitis. Hygiene procedures twice a day with properly selected products, the use of dental floss and rinses will help make recovery faster.
HOW MUCH WILL THE TREATMENT COST?
The cost of periodontal treatment will depend on the type and amount of work planned. When considering an investment in your own health, consider that treating gum disease is cheaper and better for your health than restoring a tooth lost due to untreated periodontal disease.
New direction – aesthetic surgical periodontology
Recently, such a direction as aesthetic surgical periodontics has appeared and is actively used in surgical periodontology. She deals with the correction of changes in the position of the gingival margin relative to the neck of the tooth, and gum growths. Aesthetic surgical periodontics includes a large number of new surgical techniques, depending on the clinical situation and the desired aesthetic effect.
Stomatitis
This is a group of diseases characterized by inflammation of the oral mucosa with hyperemia, swelling, and an increase in the amount of mucus in the oral cavity.
Depending on the severity and depth of the lesion, even ulcers or foci of necrosis may form in the oral cavity, sharply disrupting the general condition - fever, weakness, anxiety, refusal to eat. There are many causes of the disease: mechanical, chemical, thermal, bacterial factors. Often the cause of the disease in infancy is contaminated nipples, toys and other objects that fall into the child’s mouth. Stomatitis often develops as a result of infectious diseases (measles, scarlet fever, influenza, whooping cough, etc.). The mucous membrane of the oral cavity acquires a bright red color, becomes swollen, and tooth marks are visible on the mucous membrane of the cheeks and tongue. Saliva becomes viscous and viscous. The mucous membrane is covered with a whitish coating. The tongue is dry, swollen, often with a brown tint, chewing is painful. The duration of the disease is from 1 to 3 weeks, the prognosis is favorable.
A general preventive rule for children and adults is to maintain good oral hygiene.
ARE THERE METHODS FOR PREVENTION OF PERIODONTAL DISEASES?
- Prevention of periodontal disease consists of several simple points:
- Brush your teeth 2 times (morning and evening) after meals. Use a toothpaste recommended by your doctor to protect your gums. Use an electric toothbrush - it perfectly cleans your teeth and massages your gums.
- Do professional oral hygiene at least 2 times a year, and at the same time you can undergo an examination by a periodontist. Do not use any medications for the treatment or prevention of periodontal disease (gels, ointments, tablets, etc.) without consulting your dentist.
- Do not eat only soft and delicate foods - your teeth should receive normal, natural stress.
- Your diet should be well balanced, contain the required amount of proteins, fats, carbohydrates, and vitamins. If you are deficient in vitamins, take multivitamin complexes.
- Lead a healthy lifestyle.