Lidocaine is an effective pain reliever. Local anesthetics inhibit the ionic currents involved in the formation of the irritant, due to which the analgesic effect is achieved. Lidocaine stabilizes neuronal membranes, suppresses nerve conduction, and reduces the degree of depolarization.
When is lidocaine indicated?
The range of indications for Lidocaine solution includes the following conditions:
- Local anesthesia required for manipulations in ophthalmology, ENT practice, dentistry, and surgery.
- The use of cephalosporin group of antibacterial drugs as a solvent, the administration of which is characterized by a pronounced pain effect.
Lidocaine for injection allows you to anesthetize the desired area of skin or mucous membrane for several hours, which will be enough for medical manipulation accompanied by increased sensitivity.
How is lidocaine solution used?
The local anesthetic solution is pre-tested on a separate area of the skin, which makes it possible to assess the presence or absence of an individual negative reaction to the drug.
The dosage of lidocaine solution depends on the type of anesthesia:
- Terminal type of anesthesia involves local application of a solution (2 mg per kg of body weight), maximum 20 ml for an adult patient. The effect lasts no more than 30 minutes.
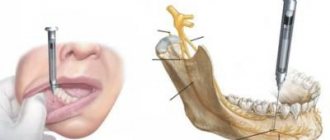
- Conduction type of anesthesia. The dosage depends on the size of the area that needs to be anesthetized. Maximum dose 20 ml.
- In ophthalmology, the solution is instilled into the conjunctival sac.
- Epidural anesthesia – 22-30 ml of solution.
- Pain relief in obstetrics and gynecology – 20-30 ml of solution.
- In childhood, the dosage is determined individually (on average 3.5-4 mg per kg of weight).
To prevent the development of side effects, the solution must be administered strictly in recommended dosages. The medication Lidocaine, the instructions for use of which contains all the necessary dosages, must be prescribed after a detailed study of the anamnesis.
Modern analogues of novocaine in dentistry -
Lidocaine replaced novocaine around the 90s. Lidocaine is 2.5 times stronger than novocaine in terms of depth of anesthesia and duration of effect, and it does not lose effectiveness when administered in the area of inflammation (for example, with purulent abscesses). Lidocaine also has a much lower incidence of side effects. But as we said above, in dentistry lidocaine is now used only in provincial medical institutions, because In terms of depth and duration of anesthesia, lidocaine is 2-3 times inferior to articaine preparations (for example, ultracaine).
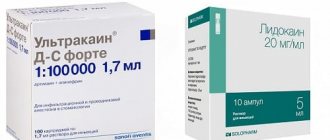
Lidocaine 2% solution in ampoules of 2 ml –
And although lidocaine is now practically not used in dentistry, in general surgery it is still one of the most widely used local anesthetics (24stoma.ru). The most popular anesthetics in dentistry today are drugs based on articaine (for example, ultracaine, ubistezin, septanest and others). For dentists, these drugs are no longer produced in glass or plastic ampoules, but in special glass carpules.
Carpule syringe and anesthetic carpules –
Each capsule contains 1.7 ml of anesthetic and is ready for use (i.e. it does not need to be opened). It is completely inserted into a special carpule syringe, into which a special double-sided needle is then screwed in from the side of the syringe nose. When you press the syringe plunger, the latter presses on the movable rubber tab located in the lower part of the carpule, which causes an increase in pressure inside the carpule and leads to the release of the anesthetic solution through the needle into the tissue.
How is anesthesia performed in dentistry?
For more information about modern anesthesia in dentistry, read the article: → Pain relief in dentistry
Adverse reactions
If used incorrectly, adverse reactions may occur:
- Dizziness, drowsiness, convulsions, sensory disturbances.
- Tinnitus.
- Changes in blood pressure, cardiac dysfunction.
- Nausea, vomiting.
- Feeling of heat, swelling at the injection site.
- Burning sensation, thrombophlebitis.
The list of adverse reactions is much wider, so it is necessary to monitor the patient’s condition after administration of the lidocaine solution.
Contraindications for the use of Lidocaine and Novocaine
Contraindications to the use of Lidocaine:
- severe liver dysfunction;
- AV block II and III degrees;
- SSSU in elderly patients;
- severe forms of chronic heart failure;
- cardiogenic shock;
- severe bradycardia;
- infection of the intended injection site;
- arterial hypotension;
- shock;
- heavy bleeding.
Novocaine is prohibited in case of excessive sensitivity to the components of the drug.
Contraindications to the use of lidocaine solution
The use of the drug is prohibited in patients with individual intolerance to the active substance. Lidocaine injections are also prohibited for use in the following conditions:
- The first few months after myocardial infarction.
- Severe cardiac pathologies with bradycardia.
- Infectious process at the injection site.
- Period of pregnancy, lactation.
- Children's age (up to 15 years).
- Convulsions due to epilepsy.
In these conditions, the use of lidocaine solution is not recommended.
Modern approaches to the management of patients with back pain
P.R. Kamchatnov
Russian State Medical University, Moscow
One of the most common clinical syndromes is pain in the lumbosacral region (back pain), caused by vertebrogenic pathology. Back pain occurs in 60–80% of the adult population and is one of the most common causes of temporary disability. Episodes of back pain occur annually in half of the working population, with individuals aged 35–55 years most commonly affected. The number of such patients is extremely high, especially in outpatient neurological settings. It is believed that in the vast majority of cases (about 90%), the duration of the pain syndrome does not exceed 6 weeks, however, in other patients the pain becomes chronic. There is a tendency towards an increase in the incidence of musculoskeletal diseases. Thus, in the Russian Federation, the number of such patients over the past 10 years (1988–1997) has increased from 7.7 to 11.2 million (by more than 40%). It should be taken into account that the actual prevalence of these diseases is probably much higher.
The main causes of back pain are degenerative changes in the spine, in particular osteochondrosis, dysfunction of the facet joints, partial tear of the fibrous ring, prolapsed intervertebral discs, in some cases complicated by the formation of a disc herniation, spondylolisthesis, spinal canal stenosis, osteoporosis. It must be taken into account that in some patients the source of pain may be inflammatory changes in the vertebrae or adjacent tissues (spondylitis, osteomyelitis, epidural abscess), including those caused by the influence of a specific pathogen (for example, Koch's bacillus). The cause of pain may be a primary or metastatic tumor of the vertebrae, meninges or spinal roots. Finally, back pain may not be associated with spinal pathology, but be reflected in a wide range of somatic diseases affecting the pelvic organs, hip joint, descending aorta, etc. The variety of causes of pain requires exceptional care when making a diagnosis and developing treatment tactics. In addition to a detailed analysis of the clinical picture of the disease and radiological examination (including the use of computed tomography - CT and magnetic resonance imaging - MRI), there is often a need for an in-depth somatic examination of the patient.
Significant risk factors for the development of intervertebral disc damage are a sedentary lifestyle with a lack of physical activity or, conversely, increased physical activity with repeated microtrauma to the spine, exposure to vibration, excess body weight, high growth, and repeated pregnancies. Production factors play a major role - long stays in vehicles, frequent hypothermia, a discrepancy between the physical capabilities of the individual and the amount of stress experienced. Congenital structural features of the skeleton (asymmetry of leg length, abnormalities in the structure of the hip joints, lumbarization or sacralization, etc.) can also be considered as factors predisposing to the occurrence of degenerative lesions of the spine. There is information about the genetic determinism of intervertebral disc damage, in particular due to impaired production of type 1X collagen.
The presence of long-term chronic pain in the back or lumbar region is closely associated with the development of depression and anxiety disorders, while the frequency of depressive disorders among patients with spondylogenic dorsopathies is 3–4 times higher than in the general population. There is a relationship between the severity and duration of the pain syndrome and the severity of subsequent violations of the motor stereotype and emotional disorders. The presence of depressive and anxiety disorders, especially in combination with pain, can not only cause a decrease in the quality of life of patients, but also lead to permanent disability. Even when acute pain is relieved, emotional disorders can persist for quite a long time, causing maladaptation of the patient.
Management of the patient in the acute period
The main objectives of managing a patient in the acute period of pain as part of spondylogenic dorsopathy are pain relief, restoration of normal spinal biomechanics, and creation of conditions for a full course of rehabilitation measures. The earliest and complete relief of pain syndrome can prevent the fixation of a pathological motor stereotype and provide the opportunity for early rehabilitation measures. In addition, timely elimination of pain provides, on the one hand, the opportunity for early involvement of movement therapy and its activation, and on the other, prevents the development of emotional disorders. Currently, the advisability of choosing a therapeutic tactic that prevents the chronicization of the pathological process is beyond doubt.
In order to eliminate pathogenic physical factors that can cause increased pain, it is recommended to provide a gentle motor regimen, completely eliminate or limit physical activity (“it’s better to lie down for three days than to be treated for a week”). It is advisable to provide a gentle regimen at home or in a neurological hospital. The patient should avoid flexor or rotational movements of the lumbar spine, especially those performed at a fast pace or with additional physical activity. If hospitalization is impossible, immobilization of the corresponding part of the spine should be ensured using orthoses, fixing belts (corsets) equipped with vertical stiffeners. In the acute stage of the disease, characterized by the presence of severe pain, it is, as a rule, inappropriate to carry out active gymnastic exercises, manual massage, as well as the use of thermal procedures and manual therapy sessions. At the same time, with relatively mild exacerbations, in the case of moderate pain syndrome, with a predominance of muscle-tonic disorders, a positive effect can be achieved by performing post-isometric relaxation.
NSAIDs and analgesics
Today, there is no doubt about the advisability of using non-steroidal anti-inflammatory drugs (NSAIDs) for the treatment of patients with spondylogenic dorsopathy. The effectiveness of this approach has been established in a number of clinical studies. A characteristic feature of the pharmacological action of these drugs is the ability to inhibit the activity of cyclooxygenase-2 (COX-2), a key enzyme in the synthesis of prostaglandins, prostacyclins and thromboxanes. The role of COX-2 is known as a major catalyst in the metabolism of arachidonic acid, which is accompanied by the formation of mediators of edema and inflammation. By influencing pain endings at the site of injury, prostaglandins increase their sensitivity to bradykinin, a peptide formed in tissues during inflammation and at the same time being a stimulator of pain endings.
However, inhibition of COX-2 activity during pain syndromes associated with varying degrees of severity of the inflammatory process is not the only analgesic mechanism of NSAIDs. The different severity of the ability to suppress prostaglandin synthesis observed in drugs of this group, the dissociation between the anti-inflammatory and analgesic effects of NSAIDs suggest the existence of other mechanisms for the implementation of analgesic effects in spondylogenic dorsopathies. In addition, no direct relationship was found between the degree of suppression of the synthesis of inflammatory mediators, on the one hand, and the analgesic activity of the drugs, on the other.
The undoubted advantages of the pharmacokinetics of drugs in this group are a short half-life, lack of accumulation and enterohepatic recirculation, and long-term accumulation in the area of inflammation. Thanks to these qualities, drugs have a good benefit/risk ratio. The rapidity of onset of the analgesic effect serves as the basis for prescribing these drugs primarily for the relief of acute pain syndromes of varying intensity. The most common drugs in this group are diclofenac, ketorolac, oxicam derivatives (piroxicam, lornoxicam), propionic acid derivatives (ibuprofen, flurbiprofen, ketoprofen, naproxen).
The widely used diclofenac is characterized by good tolerability, combined with a pronounced analgesic effect. In clinical practice, it is convenient to use a prolonged form of diclofenac retard containing 100 mg of the active substance. Food intake does not have a clinically significant effect on the absorption of the active substance from retard tablets and its systemic bioavailability. The degree of absorption is directly dependent on the dose of the drug. The average maximum concentration of the drug in plasma is achieved on average after 4 hours and persists for 24 hours.
Propionic acid derivatives have a short half-life of about 4 hours and are well tolerated with a relatively low risk of side effects. These drugs are quickly absorbed in the intestine and quickly eliminated; they do not accumulate when metabolic processes are disrupted. They have moderate inhibitory activity on prostaglandin synthesis, and therefore are inferior in their anti-inflammatory effect to diclofenac, indomethacin and phenylbutazone. In this regard, it is advisable to use them for relatively mild dorsopathies with moderate pain.
Unfortunately, the vast majority of NSAIDs have an ulcerogenic effect, which forces the question of the appropriateness of their use and the method of administration into the body to be decided in each individual case. The absence of gastrointestinal diseases allows for oral administration. It is believed that the risk of gastropathy caused by taking NSAIDs is significantly higher in people over the age of 65 years, with long-term (more than 3 months) use of NSAIDs, especially when using two or more drugs from this group, while taking corticosteroids and indirect anticoagulants and , respectively, in patients with a history of gastric ulcer. Possible risk factors are female gender, smoking, alcohol abuse, and the presence of Helicobacter pylori infection. As preventive measures to reduce the risk of damage to the gastric mucosa, proton pump inhibitors (omeprazole 20 mg once a day) or H2-histamine receptor blockers (ranitidine 300 mg per day), as well as antacid drugs, can be used.
If NSAIDs are poorly tolerated, the presence of chronic gastritis, or previous peptic ulcer disease, the use of tablet dosage forms is excluded. In this case, parenteral (intramuscular) or rectal (in the form of suppositories) administration is possible. The use of rectal suppositories is characterized by a high absorption rate (it may correspond to that of oral administration or be slightly lower). Thus, after rectal administration of 50 mg of diclofenac, its maximum concentration in plasma is achieved on average within 1 hour. Unfortunately, the threat of exacerbation of gastrointestinal pathology is not completely excluded in this situation.
Recently, transdermal forms of NSAIDs (ointments, creams, gels) have become widespread. It is necessary to clearly understand that the bioavailability of drugs when administered locally is usually an order of magnitude lower than when administered orally. A serious disadvantage of transdermal dosage forms is the low concentration of the active substance and the limited passage of the drug directly to the pathological focus. Most researchers recognize the advisability of using transdermal forms for moderate pain syndromes, while for severe pain syndromes their effectiveness is clearly insufficient. A pronounced analgesic effect of the treatment can be achieved with repeated (at least 4-6 times a day) application of the drug.
Selective COX-2 inhibitors, which provide inhibition of the synthesis of inflammatory mediators and do not affect the production of prostanoids (celecoxib, nimesulide), attract much attention. The undoubted advantage of these drugs is the relatively low risk of damage to the mucous membrane of the stomach and duodenum. However, their analgesic effect in the acute stage of spondylogenic dorsopathy is not always sufficient, which requires prolongation of the course of therapy or increasing doses of drugs.
In accordance with modern ideas about the formation of pain syndromes, an important role in the formation and regulation of pain is assigned to opioid and non-opioid analgesic systems. Based on this, it can be assumed that one of the most specific and reliable options for pain management is to influence the central mechanisms of pain formation. To reduce the severity of pain in patients with back pain, it is extremely rare to use narcotic drugs. However, in some cases, a positive result is achieved through the use of non-narcotic analgesics. One of them is acetaminophen (paracetamol), an effective pain reliever with a complex mechanism of action. There is reason to believe that analgesia with its use is achieved by increasing the threshold of pain sensitivity, although the central effect of the drug cannot be excluded. It must be borne in mind that in large doses, acetaminophen can have nephro- and hepatotoxic effects, and the risk increases with alcohol intake and other exogenous intoxications.
The timing of use of NSAIDs and analgesics is determined by the intensity of the pain syndrome; the course of their use is stopped as the effect is achieved. It should be noted that the “prophylactic” use of NSAIDs in patients with spondylogenic dorsopathies in the absence of pain is inappropriate - no convincing evidence of a preventive effect has been obtained, while the risk of complications increases significantly.
Increasing the effectiveness of the use of NSAIDs can be achieved by combining drugs that affect various parts of the pathogenesis of pain. The observed potentiation of the effect makes it possible to use relatively low doses of drugs and minimize the pharmacological load on the patient’s body. For this purpose, in some patients, intravenous drip administration of a mixture of painkillers, sedatives, and diuretics can be used. In addition to the mutually potentiating effect of adequately selected components of the “cocktail,” the psychotherapeutic effect of this method of treatment cannot be excluded.
Muscle relaxants
A combination of painkillers with muscle relaxants that reduce the severity of muscle-tonic manifestations has a good therapeutic effect. This complex can be effective for both compression and reflex syndromes. Benzodiazepine derivatives (diazepam, tetrazepam), tolperisone, and tizanidine are used as drugs that reduce increased muscle tone. Tizanidine, in addition to its relaxing effect on striated muscles, has a moderate gastroprotective effect. The mechanism of this effect is not entirely clear, although there is evidence that the drug, acting through central alpha-adrenergic pathways, inhibits the production of gastric secretions, prevents changes in glycoproteins caused by the action of acetylsalicylic acid or NSAIDs, and damage to the gastric mucosa. Considering that almost all muscle relaxants have a sedative effect to one degree or another, the patient should be informed about possible side effects - drowsiness, decreased concentration, lethargy. Often the severity of these effects limits the use of this group of drugs in outpatient settings.
Decongestant therapy
In some cases, compression syndrome is accompanied by local venous congestion, swelling of the root and surrounding tissues, which makes it advisable to include diuretics (saluretics or osmotic) and, in some severe cases, corticosteroids in the therapeutic complex. Hormonal drugs usually use prednisolone (40–60 mg per day) or dexamethasone (4–8 mg per day) for 3–5 days, followed by rapid withdrawal. The increased risk of gastrointestinal complications must be taken into account when corticosteroids and NSAIDs are used concomitantly. Epidural corticosteroids are used in a number of countries. Data were obtained on the effectiveness of this method of treatment in patients with acutely developed pain syndrome. Less justified is the epidural administration of drugs for moderate pain in the lower back and lower back, as well as for their chronic or subacute nature.
Combination drugs
A successful combination of drugs that have analgesic and anti-edematous effects, which have a positive effect on metabolism in the peripheral nerve and surrounding tissues, is the drug “Ambene”. Available in the form of a ready-to-use two-chamber syringe for injection, the first chamber of which contains 2 ml of phenylbutazone solution (375 mg) and 3.5 mg of dexamethasone, the second - 1 ml of cyanocobalamin (2.5 mg). In addition, Ambene contains lidocaine, the addition of which reduces pain directly at the injection site. Solutions are mixed immediately before use. The therapeutic effects of the components included in Ambene are potentiated, thereby ensuring a quick and lasting analgesic effect.
Phenylbutazone is a pyrazolone-type NSAID, which, by inhibiting COX activity, reduces the production of prostaglandins and has an analgesic and anti-inflammatory effect. The pronounced analgesic effect is combined with good tolerability, so the daily dose can be up to 1200–1600 mg. Dexamethasone is a synthetic glucocorticoid with powerful anti-inflammatory, antiallergic, desensitizing, and anti-edematous effects. The main clinical effects are realized due to inhibition of the release of inflammatory mediators by eosinophils, membrane-stabilizing effects, and a decrease in the number of mast cells. Cyanocobalamin (vitamin B12) is involved in the metabolism of a number of biologically active substances and has high biological activity, including in relation to metabolic processes in the peripheral nervous system.
Ambene has a pronounced analgesic effect in patients with spondylogenic dorsopathy, and is well tolerated. The drug is administered intramuscularly once a day, no more than once every 2–3 days. It should be borne in mind that individual components of the drug can cause unwanted side effects. Like other NSAIDs, phenylbutazone has an ulcerogenic effect; skin manifestations (urticaria, dry eczema) are relatively rare. Dexamethasone is characterized by a low incidence of side effects, however, it is necessary to keep in mind the possibility of reducing glucose tolerance and increasing the risk of developing erosive and ulcerative lesions of the stomach and duodenum. Based on this, Ambene should not be used in patients with acute diseases of the stomach and duodenum, impaired carbohydrate metabolism (decreased glucose tolerance), or individual intolerance to its individual components.
Relief of both compression and reflex pain syndromes can be achieved by blocking painful muscle groups or trigger points. Technically correctly performed, these manipulations are quite effective and do not cause significant complications. Care is required when performing paravertebral blocks to avoid trauma to the spinal roots. Combinations of anesthetic solution (novocaine, lidocaine) and a small dose of corticosteroid (hydrocortisone suspension, betamethasone dipropionate) are used. Local administration of drugs that have a systemic rather than local effect (antiplatelet agents, vasoactive drugs, muscle relaxants, etc.), and also do not have the ability to be deposited in tissue, is impractical. Unfortunately, the effect of blockades on pain is not lasting, and therefore there is a need for repeated manipulations.
In some cases, the use of NSAIDs, even in combination with muscle relaxants, does not have the desired positive effect. Chronic pain syndrome is accompanied by emotional disorders, in particular with a predominance of depressive reactions, which dictates the need to expand the pharmacotherapeutic arsenal. Research in recent years has convincingly demonstrated that the chronicity of pain in patients with lumbar pain is due to psychological rather than biomechanical reasons (i.e., directly related to the pathology of the spine and roots). The consequence of this is an increase in the recovery process, a sharp limitation in the possibility of motor rehabilitation of patients, and disruption of interaction in the “doctor-patient” system. The reasons that complicate the recovery process are the patient’s belief in the presence of progressive organic damage to the spine, the need to completely limit physical activity, impairment of social functions associated with the disease, orientation towards passive (medicinal, physiotherapeutic) but not active treatment (dosed physical activity, special exercises). A powerful therapeutic tool in this situation is conducting explanatory psychotherapy, developing optimistic views in the patient about the prospects for treatment, developing a behavior strategy for the future (optimal volume and nature of work and household stress, carrying out preventive measures, etc.).
Antidepressants and anticonvulsants
In this situation, antidepressants can be added to treatment, and it is advisable to use drugs that have a sedative and muscle relaxant effect (for example, amitriptyline). Carbamazepine, an effective anticonvulsant from the group of iminostilbene derivatives, has an analgesic effect. The drug inactivates sodium channels, inhibits the release of excitatory neurotransmitters into the synaptic cleft, causing a decrease in synaptic transmission. In addition to the main anticonvulsant and analgesic effect, the drug has antipsychotic and antimanic effects. It has been suggested that the positive effect of carbamazepine in patients with spondylogenic dorsopathies may be mediated by its effect on central nociceptive mechanisms and normalization of muscle tone. Dosing of the drug is carried out individually, depending on tolerability, as well as on the nature of the motor mode. Side effects (primarily drowsiness, impaired concentration) require care in selecting the dose of the drug, especially in an outpatient setting. The likelihood of these disorders increases with the simultaneous prescription of sedatives, antidepressants, and some muscle relaxants. Convincing data on the advisability of using other anticonvulsants has not been obtained, although studies of this kind are being conducted.
The complex of therapeutic measures should also include non-drug treatment methods - physiotherapy (phono- or electrophoresis of drugs, exposure to electric currents of a specially selected configuration, frequency and voltage, low-energy laser radiation). Reflexology in various modifications (traditional acupuncture, electro- and laser puncture) has an analgesic effect. It should be noted that there are significant difficulties in comparing the results of using various physiotherapeutic treatment methods, and the obvious lack of research on their effectiveness that meets the requirements of evidence-based medicine.
Currently available data indicate the existence of a significant arsenal of pharmacotherapeutic and non-drug methods for relieving pain in patients with spondylogenic dorsopathies. It seems desirable to make an individual choice of therapeutic tactics using a combination of different drugs, their dosages and routes of administration. The combined use of various treatment methods can increase the effectiveness of treatment and reduce the pharmacological load on the body. As the pain syndrome is relieved, it is absolutely necessary to use methods of restorative therapy, therapeutic exercises aimed at forming a muscle corset, strengthening the muscles of the abdominal wall and back. Equally important is teaching the patient the skills of daily physical activity - the formation of a motor stereotype that prevents the occurrence of pain.
Source: https://www.consilium-medicum.com/media/consilium/04_08/557.shtml :: Wednesday, 10-Nov-2004 21:25:33 MSK
Interaction of the solution with other drugs
Lidocaine is not recommended to be combined with the following groups of drugs at the same time:
- Analgesics of the narcotic group - threatens respiratory depression.
- Anticoagulants – increases the risk of bleeding.
- Cardiac glycosides – their effectiveness decreases.
- Novocaine group – increases muscle relaxation.
- The standard is a negative effect on respiratory function.
Lidocaine solution should be combined with extreme caution in diseases of the heart and nervous system, accompanied by systematic use of drugs.
Which is better - Lidocaine or Novocaine
To find out which drug is better to use - Lidocaine or Novocaine, the doctor assesses the patient’s condition and situation. The first drug has a profound analgesic effect. Compared to other powerful anesthetics, such as Ultracaine, Lidocaine shows an average effect. However, it has a stronger effect in dental treatment than Novocain. The latter medication is often used in situations where rapid and long-term pain relief is not required.
Lidocaine is prescribed not only for anesthesia.
The drug increases the permeability of cells to potassium, as a result of which the penetration of sodium is blocked. Thanks to this quality, the medicine is used during heart surgery and myocardial infarction.
Which is stronger
If a strong pain reliever is required, lidocaine is used. It begins to act quickly and has a long lasting effect.
special instructions
Lidocaine injection should only be done under the supervision of a physician. Treatment should be carried out under ECG control.
Before starting treatment, it is recommended to examine the level of potassium in the blood, since if its content is reduced, the effectiveness of the drug decreases.
The drug has an effect on the central nervous system, so it is not recommended to drive or engage in potentially life-threatening activities while using it.
Careful monitoring is required for patients prone to seizures, as even small doses may enhance the convulsive effect.
It is necessary to combine lidocaine with caution with those drugs that increase its bioavailability or slow down its elimination, which can be especially dangerous in case of end-stage renal failure.
With intramuscular administration of lidocaine solution, increased activity of creatine phosphokinase may be observed, which prevents the diagnosis of myocardial infarction.
Rapid administration of lidocaine solution can lead to a sharp decrease in blood pressure, with the possibility of collapse. In this case, the toxic effect of the drug with its cardiotoxic effect should also be considered.
What is the difference
To find out the difference between drugs, a comparison is required. Lidocaine is an amide compound, Novocaine is an ester compound. Esters are unstable in solutions, and when they enter the body they quickly disintegrate. Hydrolysis products often provoke allergic reactions. Amides are relatively stable and degrade slowly. In this case, allergies rarely occur.
Lidocaine differs from Novocaine in its strong analgesic effect. It is available in the form of a solution for injections, eye drops, spray, gel and transdermal patch for topical use. Novocaine has a moderate analgesic effect. It is produced in the form of injections in ampoules, rectal suppositories and infusion solution. In addition, the effects of this drug do not last long.
Lidocaine is characterized by antiarrhythmic properties, effectively anesthetizes tissue, and interacts well with other anesthetics. The drug rarely causes side effects. Novocaine has a vasoconstrictor effect, improves blood microcirculation and reduces myocardial excitability. It often leads to the development of negative reactions in the body.
The dosage of both medications is determined by the doctor, since an overdose can cause apnea, seizures, and even coma.