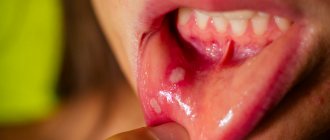
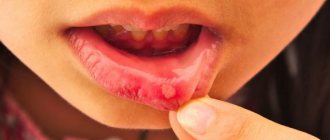
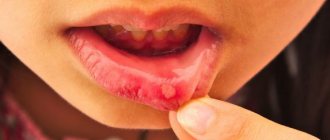
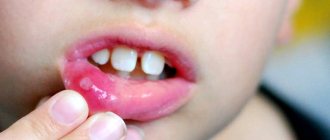
According to statistics, more than 80% of parents are faced with such an unpleasant disease in their child as stomatitis. Some people think that this is a harmless disease. Moreover, if treatment is not started on time, this will lead to complications and an increase in the duration of therapy.
Stomatitis is the general name for a disease that manifests itself in the form of ulcers on the oral mucosa. It can form on the roof of the mouth, gums, tongue, cheeks and even in the lips. Among the reasons for this occurrence are the following:
- mucosal injury;
- diseases of the gastrointestinal tract;
- poor oral hygiene;
- entry of bacteria.
Due to the fact that with any type of stomatitis the integrity of the mucosal epithelium is disrupted, in children the symptoms look the same: the formation of plaque, erosions and ulcers, redness, pain, bad breath, swelling.
Types of diseases that most often occur in young patients:
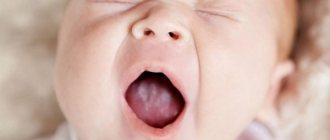
- candidiasis - infants are often susceptible to this variety. The reason is the active proliferation of the fungus of the genus Candida. A white “curdled” coating appears in the oral cavity;
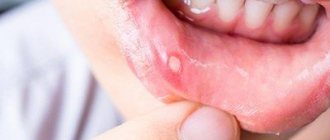
- aphthous - small reddish ulcers appear;
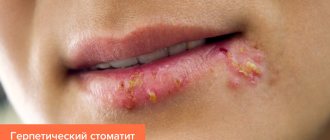
- herpetic - characterized by a large number of rashes that are filled with liquid. They combine and turn into erosion with a white coating;
- angular - when jams appear in the corners of the lips.
Causes of stomatitis
In children, as in adults, stomatitis can be caused by viruses, fungi, bacteria, allergies and injuries. About six months after birth, the child loses the immunity received from the mother, the protective power of the immune system changes, and the child’s body becomes more susceptible to infections. The oral mucosa in children is more delicate and easier to injure; children also more often “bite” their cheeks after dental treatment due to a temporary loss of sensitivity after anesthesia, which causes traumatic stomatitis.
Children are not always motivated to brush their teeth, so poor hygiene can also cause stomatitis.
With the following diseases, stomatitis is observed in children much more often: chronic tonsillitis, diabetes mellitus, heart defects, chronic hepatitis.
Diagnostic features
A dentist can detect stomatitis during the first visual examination. But in controversial cases, laboratory tests may be required. Thus, bacterial inflammation may require identification of the causative agent of the disease and its sensitivity to antibiotics. A scraping and/or virological study will help determine the cause of the disease and prescribe appropriate treatment.
If a combination of several ailments with a similar picture is suspected, as well as if the child’s general well-being deteriorates, laboratory tests of blood and urine and consultations with other specialists may be prescribed.
Sometimes stomatitis can be the first manifestation of systemic diseases, general somatic pathology, for example, diabetes mellitus or malignant neoplasms. Therefore, a timely visit to the doctor is extremely important.
Classification of HRAS (chronic recurrent aphthous stomatitis)
| CLASSIFICATION | A COMMENT | ||
| classification: | According to the degree of damage to the mucous membrane: | a comment: | 1) Superficial (catarrhal, fibrinous) 2) Deep (ulcerative, necrotic) |
| classification: | According to the clinical course: | a comment: | 1) acute 2) chronic |
All types of stomatitis occur in children, but the most common are: herpetic, candidal and traumatic stomatitis.
Acute herpetic stomatitis
It occurs most often, and mainly affects children from 10 months to 3 years.3 The appearance of rashes is preceded by inflammation of the lymph nodes.
With a mild form
In acute herpetic stomatitis, the temperature rises to 37-37.5°C, the general condition is satisfactory, slight swelling and redness may occur on the gums, then up to six blisters appear, which burst with the formation of painful aphthae surrounded by a red rim.
Afta is a round-shaped erosion. Aphthae may merge together. The rash appears once, and after 1-2 days the erosion gradually heals.
Moderate form
Acute herpetic stomatitis is characterized by deterioration of the child’s well-being, weakness, and headache. The child is capricious, has no appetite, the lymph nodes are enlarged and painful, the temperature rises to 38-39°C, the symptoms resemble ARVI. The oral mucosa is swollen, reddened, rashes appear (bubbles, then erosions) of 10-15 pieces, and often there are rashes on the face. Salivation increases, and gingivitis appears (inflammation of the gums, accompanied by bleeding). The rash may appear several times, i.e. after the old ones heal, new ones appear. Healing of erosions takes up to 4-5 days. Bleeding gums and swollen lymph nodes persist for some time after the erosions have healed.
Severe form
It begins as an acute respiratory viral infection, there is pain in the muscles, joints, tachycardia and bradycardia (increased and slow heartbeat), and nosebleeds may even be observed. In this form, the temperature is high up to 40°C, gingivitis is pronounced, the mucous membrane is bright red, swollen, the child’s lips are dry, the mucous membrane of the eyes is swollen, reddened. The rashes constantly appear again, their number can reach 100. Rashes often appear around the mouth, on the eyelids, on the mucous membranes of the eyes, between the fingers, on the earlobes. Simple gingivitis turns into ulcerative (a more severe form of gum inflammation, with the formation of ulcers), salivation increases, and bad breath appears. Recovery is long and hospitalization is often required.
Kinds
Today, 8 types of stomatitis can be diagnosed:
- bacterial;
- aphthous - manifests itself when immunity decreases due to gastrointestinal diseases and anemia;
- herpetic – occurs due to the herpes virus;
- viral;
- angular;
- allergic – a reaction to an allergen entering the child’s body;
- traumatic - the cause may be an accidental bite of the lip with teeth or scratches on the gum;
- fungal – infection of the oral cavity by fungi of the genus Candida.
All types of stomatitis can occur in childhood. However, from birth to 3 years, children are especially susceptible to aphthous, candidal, herpetic and allergic types. During the period of active growth of baby teeth, traumatic stomatitis often appears, caused by rupture of the soft tissue of the gums.
Note! Stomatitis does not always occur on its own. Quite often, rashes in the mouth are a sign of other diseases, so before treatment it is necessary to carry out a series of diagnostic measures to discover the exact cause.
Symptoms
The classic clinical picture for diagnosing stomatitis includes the following symptoms:
- swelling of the mucous membrane;
- the appearance of a white or yellowish coating;
- bad breath;
- dryness or excessive salivation;
- enlarged lymph nodes and increased temperature.
Stomatitis in children has similar and different symptoms. Each type of disease has its own differences in manifestations.
With allergic stomatitis, minor ulcerative lesions appear on the palate, gums, cheeks, and lips. They pass as soon as the irritant can be identified and removed. With aphthous, even one spot with a diameter of up to 1 cm may appear in the mouth. Its outer part is covered with a film, the ulcer is yellow, and its edges are inflamed. If stomatitis is herpetic, then the mucous membrane is affected by numerous rashes that merge into one large wound. These are blisters with clear liquid and are extremely painful. Often the herpes virus causes a deterioration in the general condition of the child’s body, accompanied by body aches and high fever.
The most common type of stomatitis in a child’s mouth is candidiasis. Its common name is thrush. 9 out of 10 parents have encountered this phenomenon at least once. It is characterized by the appearance of a white cheesy coating on the tongue, gums, and cheeks of the baby. It is often observed after completing a course of antibacterial therapy or as a consequence of infection of the mother’s nipples by Candida fungus. Candidiasis can also be caused by poor hygiene.
On a note! Regardless of the type of stomatitis, its treatment should be comprehensive and begin immediately after the first signs of damage to the oral cavity are detected!
Treatment options
How to cure stomatitis in a child? It’s worth noting right away that you can’t prescribe medications to your baby yourself. Only the pediatrician makes a diagnosis and makes recommendations for therapy. Attempts to overcome the disease on your own can lead to a worsening of the little patient’s condition. To determine the causative agent of the inflammatory process, a scraping is made and a virological study is carried out.
For stomatitis in children, what treatment will be most effective? Only those therapeutic measures will help that will affect the disease comprehensively, eliminating both the cause and external manifestations.
Medicines
When an accurate diagnosis is established, dentists prescribe medications for the treatment of stomatitis in children. They are conventionally divided into symptomatic and special.
The purpose of the first is to eliminate the symptoms that accompany the disease. For this purpose the following is prescribed:
- vitamin complexes to strengthen the body;
- antiviral drugs that fight viruses;
- antipyretic and anti-inflammatory drugs;
- anesthetic gels;
- ointments and solutions for treating the oral cavity.
- need to drink plenty of fluids
- gentle diet (exclude sour, salty, spicy)
Candidal stomatitis is treated with special pharmaceuticals that contain substances that kill the fungus. Creams suitable for internal use are prescribed. If an allergic type is detected, the pediatrician will add antihistamine drops or tablets to the general list. If the rash is caused by the herpes virus, you cannot do without taking antiviral drugs, as well as local treatment of the mucous membranes with antiherpetic ointment.
Attention! The entire oral cavity needs to be treated, since pathogens are found everywhere on the mucous membrane. They are not visible to the naked eye, but if they remain in the mouth, they will continue to spread and the treatment will be delayed.
Folk remedies
Have you noticed stomatitis in a child and don’t know how to treat it? Drug therapy can be supplemented with the use of traditional medicine. Compositions prepared from natural ingredients are used to treat stomatitis in children over 2 years of age.
The following formulations are suitable for treating mouth ulcers.
Soda and salt
0.5 tsp each Dissolve the components in warm water. Rinse your mouth with the solution 3-4 times a day after meals. Baking soda relieves inflammation and disinfects well. The same composition, only diluted with water to a mushy consistency, can be used to clean off plaque from fungal stomatitis using a finger wrapped in gauze.
Honey and aloe
The leaf of the plant is ground to a puree, and the same amount of natural honey is added to it. Apply to affected areas three times a day.
Chamomile with honey
Dried flowers are brewed in the proportion of 1 tbsp. for 250 ml of boiling water. Add 2 tsp to the cooled broth. honey Rinse your mouth with warm liquid 2-3 times a day.
Rinses can be prepared from other ingredients:
- sage;
- rosehip;
- St. John's wort;
- oak bark;
- flaxseeds;
- yarrow;
- calendula;
- propolis tinctures.
Lotions of essential oils help a lot.
Important! Folk remedies can only be used after consulting a pediatrician!
How to prevent stomatitis
To reduce the risk of getting an infection in your mouth, you should:
- regularly wash toys, hands, pacifiers, bottles;
- carry out wet cleaning and ventilate the room where the baby spends his leisure time;
- strengthen the immune system: strengthen the child, give vitamins, maintain proper sleep and wakefulness;
- provide a balanced diet;
- fight the bad habit of biting nails or other objects (pencils, pens, rulers);
- Make an appointment with the dentist twice a year for a routine examination.
Any disease should be treated in a timely manner, otherwise negative consequences cannot be avoided. Carefully examine the child’s oral cavity at the first complaints. When stomatitis occurs in infants, the first symptoms include behavioral changes, crying, and refusal of the breast or bottle. Children aged 1 year and older will be able to independently point out to their parents the source of discomfort. Get treated promptly and be healthy!
Enteroviral vesicular stomatitis (arm - leg - mouth)
Caused by enteroviruses. It also occurs in adults, but in 95.7% of cases children are affected.6 It is characterized by seasonal occurrence (summer - autumn) and group incidence.4 It is observed mainly in children under 10 years of age. Vesicular stomatitis is contagious, so it is recommended to use separate utensils and hygiene products. Characteristics for this disease: temperature 37.5-38, weakness, headache, muscle pain, rash on the palms, soles, as well as blisters on the hard palate and pharynx, which then turn into erosions that are almost not painful.
Acute pseudomembranous candidal stomatitis (thrush)
Acute pseudomembranous candidal stomatitis (thrush) occurs:
- Light shape
- Medium-heavy forms
- Severe form
The main symptom of the disease is a white or yellow coating.
With a mild form
The plaque is located in islands, most often on the tongue and cheeks. Children are restless, sleep poorly, and suck the breast sluggishly. Older children may complain of a burning sensation. The plaque is easily removed; underneath there is a bright red mucous membrane. The disease lasts no longer than 7 days.5
Moderate form
The plaque is located on the cheeks, tongue, hard palate, and mucous membranes of the lips. Under the plaque, erosions form, which sometimes bleed. The plaque is more difficult to remove. Lymph nodes are sometimes enlarged and painful. The duration of the disease is 10-15 days, there are relapses.
Moderate form
The plaque is dirty gray, almost cannot be removed, and is located on the tongue, cheeks, soft palate, tonsils, pharynx, and mucous membranes of the lips. Cheilitis appears in the corners of the mouth - inflammation of the lips. The oral mucosa is dry and inflamed. The child’s health is impaired, the child refuses to eat, and the temperature rises. Lesions in the genital area, neck folds, and between the fingers are also common. The disease is long-term, with frequent relapses.
What happens if stomatitis is not treated?
Some parents do not take their child’s stomatitis seriously, they say, “it will go away on its own.” Such an attitude towards the baby’s health can lead to serious consequences. Without treatment, the infection can spread to the skin of the face. There is also a high risk of secondary infection. And this already threatens general intoxication of the body, damage to the nervous system, etc., even death. Therefore, doctors strongly recommend that if symptoms of the disease are detected, show the child to a specialist in order to avoid negative health consequences.
Bacterial stomatitis in children
Necrotizing ulcerative stomatitis is more common in weakened children and is caused by fusobacteria and spirochetes. May be a sign of periodontal disease (progressive destruction of periodontal tissue). It is characterized by the appearance of painful ulcers, weakness, gingivitis (inflammation of the gums), enlarged and painful lymph nodes, difficulty eating, speaking, and bad breath.
Often, erosions in traumatic stomatitis can become infected through dirty hands, toys and other objects, then bacterial stomatitis develops, so it is important to pay attention to antiseptic treatment.
Traumatic stomatitis in children
A specific form of traumatic stomatitis in children is Bednar's aphthae . This is a traumatic erosion of the oral mucosa. In children, unlike adults, the mucosal epithelium consists not of four layers, but of two, so it is easily injured. The cause may be early teething, a rough nipple from the mother, or a long nipple on the bottle. Erosion is most often located in the middle of the palate or opposite the cutting edge of the teeth. The child begins to refuse food, cries, and sleeps poorly.
Traumatic stomatitis also occurs in children when wearing braces. Erosions have uneven edges, are painful, and are usually located on the mucous membrane of the cheeks and lips, less often on the tongue.
Features of treatment
As is often the case with diseases that are at the intersection of several areas of medicine, inflammatory lesions of the oral mucosa are one of the least studied areas of dentistry. Therefore, several specialists can be involved in the treatment of stomatitis in children in the mouth: pediatrician, dentist, dermatologist, immunologist-allergist, otolaryngologist, etc. This is especially convenient when you go to a multidisciplinary clinic.
Self-medication of stomatitis is unacceptable, and although it is now easy to find ready-made treatment regimens and folk recipes, it is important not to experiment with the baby’s health.
Conservative treatment is mainly used, which involves treating the underlying cause of the disease. Your doctor may prescribe the following medications:
- antibacterial drugs (systemic and local in the form of ointments): for bacterial inflammation;
- antiviral agents for herpes and other types of viral stomatitis;
- antifungal drugs for fungal diseases;
- antihistamines - both for allergic origin of stomatitis, and as part of complex therapy to reduce swelling and itching;
- symptomatic drugs - anti-inflammatory, analgesic, antipyretic.
Treatment of candidal stomatitis in infants should be carried out with caution. At the same time, it is important to pay attention to your health; sometimes the cause of such a disease can be insufficient breast hygiene during lactation.
Often, only local remedies are sufficient, but make sure that the entire oral cavity is treated with the rinse - inflammatory agents can be found on the entire surface of the mucous membranes. Healing applications can be used to a limited extent, only on areas of inflammation.
Treatment of stomatitis of any kind in children involves strict adherence to a diet. The diet should be gentle, it is important to avoid salty, spicy, sour foods and drinks, serve the child warm meals, and limit the consumption of sweets.
If traumatic stomatitis occurs, the doctor will prescribe medications to speed up healing. However, it is very important to prevent re-injury. If it was caused by sharp edges of a tooth or filling, this cause should be eliminated. The doctor will suggest grinding off the filling or replacing it, and will also choose the appropriate option for restoring the shape of the crown in case of chips and cracks.
Drug-induced stomatitis
Occurs when there is an allergy to a drug. Often, allergies can occur to antibacterial, antimicrobial drugs, vaccines, iodine. The mucous membrane is red, swollen, the lips and tongue also often swell, blisters appear, which burst, leaving erosion. The gums are inflamed and bleed when touched. General manifestations are possible, such as urticaria, nausea, vomiting. In severe cases, anaphylactic shock occurs (an emergency condition manifested by decreased blood pressure, shortness of breath, fainting, suffocation), Quincke's edema (an atypical reaction of the body, manifested by rapid and severe swelling)
Both conditions are extremely dangerous and require immediate action and calling an ambulance!
Prevention of stomatitis in children
In children's groups, infections spread especially quickly. Therefore, if a child is infected with the herpes virus, he needs to stay at home until he recovers. Children who have been in contact with sick people should use antiviral ointments for 5 days.
If a pregnant woman has herpes or candidiasis, she should treat it before giving birth. If you have the herpes virus during the period of illness, you should use separate utensils, do not kiss children, and wear a mask.
Kindergartens and other preschool institutions must be cleaned and objects, including toys, must be treated with disinfectants.
To avoid allergic reactions, you should seek help from an allergist to identify existing allergies.
It is worth preventing a decrease in immunity; hardening works especially well in childhood. It is worth limiting your intake of fast carbohydrates, because... they create a favorable environment for the development of candidiasis. An important point is the proper nutrition of the child; regular intake of vitamins, especially vitamin C, is essential.
Tantum® Propolis
For children over 14 years of age , you can use Tantum® Propolis lozenges; they contain a lot of vitamin C, which will strengthen the immune system, and propolis has an anti-inflammatory effect, preventing the occurrence of infections.7
Find out more
Prevention of Bednar's aft is preparing the breasts for feeding, using special creams to soften the skin, prevent cracks, and it is also worth choosing the right bottle. In case of injury due to braces, you need to use orthodontic wax; here it is important to prevent the wounds from becoming infected, so it is better to treat them with antiseptic solutions and sprays.
Tantum® Verde spray will relieve pain at the site of injury and its antiseptic effect will prevent infection.8,9
What do doctors advise for home care?
The specialist makes a diagnosis and prescribes treatment, and the implementation of all instructions falls entirely on the shoulders of the parents. Caring for a small child with stomatitis contains many nuances. For example, during this period you should feed your baby only warm food with a mushy consistency, excluding citrus, sour and spicy foods. After eating, be sure to rinse your mouth. If the baby is still very small, then after eating you should give him a little boiled water to drink. Treatment of the oral cavity and application of gels prescribed by a doctor should be done with a special fabric fingertip or a finger wrapped in a bandage (the bandage should then be thrown away).
Important: self-medication is dangerous. Only a doctor can correctly diagnose and give the correct therapeutic recommendations.