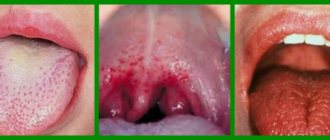
It's no secret that smoking causes irreparable harm not only to the lungs, but also to other organs and systems of the body, and is the cause of the development of many pathological processes. The bad habit of “blowing smoke” very often becomes the cause of serious diseases of the oral cavity, namely stomatitis, also called smoker’s leukoplakia.
Stomatitis is an inflammation of the oral mucosa, therefore, in addition to smoking, other factors also play an important role: dietary habits (love of spicy, sour, hot foods), consumption of strong alcoholic beverages, taking certain medications, vitamin deficiencies, some allergic reactions, etc. Tobacco smoke destroys beneficial bacteria from the surface of the mucous membrane, the microflora is disrupted and stomatitis forms. Despite the fact that stomatitis is a disease that occurs in every second baby (of course, for other reasons), heavy smokers should not let the situation take its course, as this can be extremely dangerous. Therefore, treatment must be carried out in a timely manner.
Dentists at the Dudko and Sons clinic recommend taking the symptoms of stomatitis in adults seriously. Because if the irritating factor is not eliminated for a long time and proper treatment is not followed, the disease can transform into a malignant form. Tobacco smoke contains a large number of harmful substances: nicotine, tar oils, hydrocyanic acid, hydrogen sulfide, ammonium, carbon monoxide, phenols. Nicotine itself, when smoked, does not have a significant effect on the mucous membranes of the oral cavity and respiratory tract, but purine, which is formed during its destruction, is a very dangerous substance that has a high carcinogenic effect. Nicotine stomatitis occurs in 13% of patients with various dental diseases. Their refusal of treatment or failure to properly follow the doctor’s recommendations can lead to serious complications and even oral cancer.
Features of nicotine stomatitis in adults
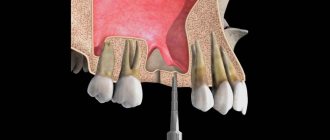
Inflammation of the oral cavity, which developed as a result of regular smoking, has its own characteristics. Namely, the main focus of inflammation is located in the palate. This is due to the fact that when inhaling, it is the palate that suffers the most, falling under the stream of tobacco smoke. Fortunately, our body is designed in such a way that over time a protective mechanism is triggered - the normal epithelium at the site of chronic inflammation begins to be replaced by denser and rougher, keratinized epithelial tissue. However, such a defensive reaction does not always have time to develop. Often ulcers appear at the site of inflammation, which can be complicated by the addition of a bacterial infection. Inflammation can also spread to the gum mucosa and affect the salivary glands.
How smoking destroys teeth
Smoking is a risk factor for the development of dental diseases. This is a habit that has an extremely negative effect on the condition of the organs and tissues of the oral cavity. The mucous membrane of the smoker's mouth, tongue, and gums is exposed to several unfavorable factors: high temperatures, irritating combustion products and toxic resins. During smoking with warm smoke, various ammonia compounds, pyridine bases, methane, methyl alcohol, phenols, senyl acid, carbon monoxide, and nicotine enter the oral cavity. (Fig.1)
Fig.1. cigarette combustion products.
Smoking can be considered as the action of a constant traumatic factor on the organs and tissues of the oral cavity. A physical and chemical irritant causes responses in the cells of the mucous membrane that appear as chronic inflammation - the formation of erosions, ulcers (minus tissue) or the formation of keratinization, the layering of new tissue (plus tissue).
Visible changes can manifest themselves in the appearance of diseases such as smoker's melanosis, smoker's leukoplakia, chronic lip injury and others. Diseases of the oral mucosa caused by smoking under unfavorable conditions can become malignant. The risk group includes patients who smoke more than a pack of cigarettes per day with an experience of more than 8 years, and the high-risk group includes patients who smoke a pack of cigarettes per day and drink alcohol more than 1 liter per week or have a “hangover syndrome” of more than 1 once a week. For patients at risk, there is a method for early diagnosis of oral cancer - the Visitlight test. (Fig. 2)
Rice. 2. Early diagnosis method “Visilyight” system.
Dark plaque on teeth - on the inner surface of predominantly the lower teeth, and subsequently on the labial surface of these teeth, a dense dark plaque appears, caused by the deposition of cadmium sulfate on the teeth, which is formed during the process of smoking and the interaction of combustion products with salivary proteins produced by the mandibular and sublingual glands. (Fig. 3).
Rice. 3. Plaque on the teeth of smokers.
Unpleasant odor (halitosis) is caused by the accumulation in saliva, on the surface of the root of the tongue and in the soft plaque on the teeth of gaseous combustion substances and sulfurous waste products of special bacteria. The accumulation of gaseous products on the organs and tissues of the oral cavity seriously alters the oral mucosa, increasing the risk of developing pathological processes (autoimmune diseases, viral, malignant formations).
Dry mouth – due to high temperatures, the oral mucosa “dries out”; over time, due to the toxic effect of smoke, the number of small salivary glands decreases. Such changes become irreversible, and dentists diagnose xerostomia, and patients experience symptoms of oral burning and changes in taste.
Gingivitis and periodontitis in smokers . Smokers are particularly susceptible to developing diseases such as gingivitis (inflammation of the gums) and periodontitis (inflammation of the gums and bone surrounding the tooth). In people who do not smoke, signs of the onset of gum problems are the appearance of bleeding - a signal of inflammation. In smokers, nicotine constricts the end blood vessels and, as a rule, the gums do not bleed. At the same time, nicotine and other toxic products weaken the defense cells in the gum tissue and the destructive process asymptomatically affects the deeper tissues of the gums and bones. The patient does not feel pain and is not bothered by bleeding, so he seeks treatment when the process already has excessively large bone defects and severe tooth mobility. Thus, nicotine causes a euphoric state and therefore painful dependence, compresses end blood vessels (impairs circulation), changes the mucous membrane, and kills defense cells. Treatment of periodontitis in patients without smoking cessation is not effective. (Fig. 4).
Rice. 4. Condition of periodontal tissues in smokers.
Melanosis of smokers - manifests itself in the form of a diffuse brown spot on the mucous membrane of the lip, gums, cheeks, palate, and floor of the mouth. Melanosis is often accompanied by brown plaque on the teeth and bad breath. Melanosis itself is not oral cancer, but other areas of the mouth may have severe changes in the lining of the mouth. (Fig. 5, 6).
Rice. 5. Melanosis of smokers on the buccal mucosa
Rice. 6. Melanosis of smokers in the lateral part of the soft palate.
Leukokeratosis of smokers - the disease manifests itself in people who smoke cigarettes to the ground. Leukokeratosis develops on both surfaces of the lips at the point of contact with the cigarette and a thickening appears at the place where the cigarette is held. Usually occurs in the elderly. If erosion appears at this site, its transformation into cancer should be excluded. (Fig. 7).
Rice. 7. Leukokeratosis of smokers on the mucous membrane of the lip.
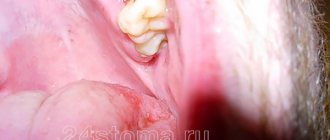
Nicotine stomatitis - manifests itself at the beginning of the formation of the smoking habit by redness of the palate, dilation of the ducts of small salivary glands in the palate, and with continued smoking over the years, the mucous membrane of the palate and tongue thickens, a “whitish” color appears and a appearance reminiscent of “cobblestones”. The cause is chronic irritation from high temperatures from pipe and cigar smoking. (Fig. 8).
Rice. 8. Nicotine stomatitis.
Smoker's leukoplakia - manifests itself on the mucous membrane of the cheeks, under the tongue, on the inner surface of the lip as a painless white thickening with a grooved surface. It is observed already in the early stages of developing a bad habit. Refers to precancers. Such changes are associated with the carcinogenic effect of nitrosamines contained in tobacco. (Fig. 9).
Rice. 9. Leukoplakia of the floor of the mouth and lower surface of the tongue.
Smoking and delayed healing
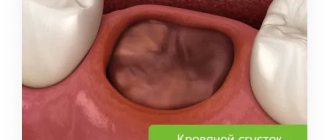
Smoking negatively affects the healing of wounds in the mouth. This is due to decreased blood flow caused by nicotine and dry mouth. Do not smoke after you have had surgery, including tooth extraction! If, however, you continue to abuse tobacco, your risk of developing alveolitis, or dry socket, increases. After extraction, a blood clot forms in the socket of the extracted tooth, protecting the bone and nerve endings. However, smoking interferes with successful healing and prevents the formation of a blood clot, leaving the bone and nerve endings vulnerable. This can lead to infection and severe pain, bad breath and an unpleasant taste.
The negative effects of smoking are considered reversible if the patient stops smoking, but this will require a long period. It is believed that the smoking factor loses its effect on the occurrence of malignant tumors only 10 years after stopping tobacco consumption.
Rice. 10. Anti-tobacco campaigns in Singapore and India
We, dentists, see every day the negative impact of smoking on the condition of teeth and oral tissues, which is why we consider it advisable to support anti-tobacco campaigns and suggest making a note on the medical history - “SMOKER”, since these are patients leading a “deadly lifestyle”.
Treatment for stomatitis caused by smoking?
Some people consider stomatitis a companion to smoking and are convinced that it does not need treatment. Unfortunately, this is a dangerous misconception. When the disease passes into the chronic stage, it is complicated by the appearance of ulcers, and this is an excellent soil for the proliferation of pathogens and the development of pathologies.
Therefore, when a problem arises, most of us wonder how to treat stomatitis? First of all, you need to quit smoking, thereby allowing the palate to heal and become covered with healthy tissue. Under no circumstances should you let the situation take its course, do not self-medicate and see a doctor. It is imperative to carry out therapeutic treatment of the gums and sanitation of the oral cavity. You can use topical preparations and various gels.
Make an appointment or consult
Links[edit]
- Rapini, Ronald P.; Bologna, Jean L.; Iorizzo, Joseph L. (2007). Dermatology: 2-volume set
. St. Louis: Mosby. ISBN 978-1-4160-2999-1. - ^ B s d e g h i JK Scully S (2013). Oral and maxillofacial medicine: basics of diagnosis and treatment
(3rd ed.). Edinburgh: Churchill Livingstone. item 287. ISBN. 9780702049484. - ^ ab Gnepp, Douglas R. (2009). Diagnostic surgical pathology of the head and neck (2nd ed.). Philadelphia, PA: Saunders/Elsevier. ISBN 9781437719512.
- ^ B s d e Vellappally, S; Fiala, Z; Smejkalová, J; Jacob, V; Somanathan, R. (2007). "Systemic and oral diseases associated with smoking". Acta Medica (Hradec Kralove) / Universitas Carolina, Facultas Medica Hradec Kralove
.
50
(3): 161–6. DOI: 10.14712/18059694.2017.76. PMID 18254267. - ^ a b James, William D.; Berger, Timothy J.; and others. (2006). Andrews' diseases of the skin: clinical dermatology
. Saunders Elsevier. item 800. ISBN 978-0-7216-2921-6. - ^ B s d e e Werning, John W. (2007). Oral cancer: diagnosis, treatment and rehabilitation. New York: Tim. paragraph 12. ISBN 9781588903099.
- ^ a b c d G. Taibos; K Crews (July 28, 2008). "Changes in the mouth associated with tobacco use" (PDF). American Journal of Medical Sciences
.
American Academy of Oral Medicine. 326
(4):179–82. DOI: 10.1097/00000441-200310000-00005. PMID 14557730. S2CID 40189451. Retrieved August 31, 2013. - ^ B s d e e Traister N. S., Bruha J. M. (2010). Clinical Oral Medicine and Pathology
. New York: Humana Press. paragraph 46. ISBN 978-1-60327-519-4. - ^ abcdefgh "Frictional, Chemical and Thermal Keratoses, from Bond's Book of Oral Diseases, 4th Edition". Maxillofacial Center for Diagnostics and Research. Retrieved September 1, 2013.
- ^ abc Laskaris, George (2006). Pocket Atlas of Oral Diseases (2nd ed.). Stuttgart: Thieme. ISBN 9781588902498.
- Kahn, Michael A. Major oral and maxillofacial pathologies. Volume 1. 2001.