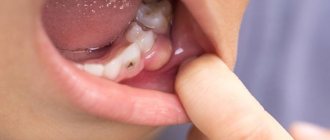
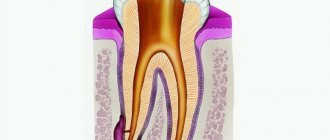
Bartholinitis is an inflammation of the large Bartholin gland. The Bartholin gland, in turn, is a paired organ that is located in the subcutaneous fatty tissue of the labia majora. When a large gland in the vestibule of the vagina becomes inflamed, microorganisms affect the excretory duct of the gland (canaliculitis), as well as the gland itself.
The main function of the Bartholin gland is to produce secretions that maintain constant moisture in the vagina. What is it for?
This secretion is released in large quantities during arousal during sexual intercourse to facilitate penile insertion. In addition, secretion is very important during childbirth. Thanks to it, the vaginal muscles stretch well and the baby can be born without damaging the vaginal walls. If the Bartholin gland does not produce secretions in the required quantity, the vagina will become dry - discomfort, itching and burning in the perineum and pain during sexual intercourse will appear. Normally, this is only possible during menopause due to the age-related decrease in female estrogen hormones.
Causes of bartholinitis:
Bartholinitis occurs due to infection in the Bartholin gland through a narrow opening of the excretory duct on the inner surface of the labia minora. Once deep into the gland, microorganisms actively multiply. This leads to inflammation and suppuration of the Bartholin gland.
Not all genitourinary infections cause bartholinitis. In the vast majority of cases, bartholinitis is provoked by sexually transmitted infections. Most often it is gonorrhea, less often - trichomoniasis and chlamydia.
Bartholinitis of nonspecific etiology is extremely rare - in this case, the causative agent is bacteria - staphylococci, Escherichia coli, streptococci, and so on. This is possible if personal hygiene rules are not followed. It should also be taken into account that even in the presence of sexually transmitted infections, bartholinitis does not develop in everyone and not always.
Immunity plays an important role in the development of the disease: if it is weakened, the chances of developing bartholinitis increase.
Depending on the clinical course of the disease, bartholinitis can be acute or chronic. Acute bartholinitis is characterized by the formation of a true or false abscess of the Bartholin gland (a limited focus with pus).
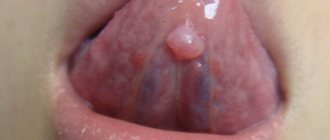
When a false abscess forms, the excretory duct of the gland first becomes inflamed (“canaliculitis”, in scientific terms). The skin over the site of inflammation turns red and swells. If you press on the inflamed area, pus will come out. Next, a blockage of the excretory duct of the gland occurs and pus is no longer released, but accumulates in the Bartholin gland. Because of this, the gland is greatly stretched and protrudes, forming a painful “bump”-shaped formation. During movements - when walking, running, during sexual intercourse - the pain intensifies, and a burning sensation appears in the perineum. Sometimes body temperature rises slightly. If you do not contact a gynecologist for a long time, the disease becomes chronic.
With a true abscess, the infection penetrates directly into the Bartholin gland, and the parenchyma of the gland melts. In this case, the symptoms of the disease are more pronounced than with a false abscess. The labia majora and minora become very swollen. The body temperature rises to more than 38 degrees, the inguinal lymph nodes enlarge, chills, weakness, and “pulsating” sharp pain in the labia majora appear. Spontaneous opening of the abscess with the release of yellow-green pus is possible, which leads to a weakening of the symptoms of the disease. But if left untreated, the inflammation recurs again and gives complications, or, like a false abscess, becomes chronic.
In the chronic form of bartholinitis, the symptoms of the disease temporarily subside and worsen again. Instead of an abscess, a cyst (liquid formation with inflammatory exudate) forms in the gland.
With any form of bartholinitis, you should never self-medicate or try to squeeze out an abscess or cyst - this can lead to blood poisoning . If such symptoms occur, you should immediately consult a gynecologist.
Complications of hidradenitis on the labia
Treatment of hidradenitis at any stage in our clinic is usually highly effective.
If timely and adequate treatment is not carried out, hidradenitis on the labia can lead to a number of complications:
- If the abscess cavity is not opened in a timely manner, the pus may spread deep into the tissues. An abscess of the soft tissues of the genital organs develops.
- Decreased immunity and the presence of severe concomitant diseases can lead to the development of an abscess or phlegmon in the pelvic cavity.
- Penetration of a pyogenic infection into the bloodstream can cause the development of thrombosis of the veins of the lower extremities, iliac veins and pelvic veins.
- In severe cases, when the pathological process is at an advanced stage and against the background of severe immunodeficiency, sepsis and infectious-toxic shock can develop.
Diagnosis of the disease is usually made on the basis of clinical data. If you seek medical help in a timely manner, the prognosis of the disease is usually quite favorable.
Diagnostic methods in surgery:
- Doppler in surgery
- Colonoscopy
- Angiography
- CT scan
- Gastroscopy
- MRI
- Abdominal ultrasound
- X-ray
- Endoscopy
Prices:
| Code | Name of service | Prices |
| 1 | Initial appointment | 1200 |
| 2 | Repeated appointment | 900 |
| 3 | Calling a surgeon to your home | 3500 |
| 4 | Abdominal ultrasound | 2200 |
| 5 | Ultrasound of veins and vessels | 2400 |
| 6 | Doppler 2-3 trimester | 1200 |
| 7 | Rectoscopy | 1500 |
Diagnosis of bartholinitis:
Diagnosing bartholinitis is not particularly difficult. The doctor will be able to make a diagnosis during examination at the first appointment. In the presence of an abscess, swelling and redness of the Bartholin gland is determined; palpation of the formation causes sharp pain. In the chronic form of bartholinitis (in the presence of a Bartholin gland cyst), a tumor-like formation is detected, painless on palpation. In addition to the examination, the following tests must be taken:
- a regular vaginal smear;
- PCR diagnosis of major sexually transmitted infections (chlamydia, gonorrhea, trichomoniasis, mycoplasmosis, ureaplasmosis, herpes, human papillomavirus);
- bacteriological culture of vaginal discharge to establish sensitivity to anitibiotics;
- bacteriological examination of pus when an abscess ruptures (or the secretion can be obtained from the excretory duct of the gland by light pressure).
Differential diagnosis
Includes cystic and solid lesions of the vulva, such as epidermal inclusion cyst, hidradenoma papilliferum and lipoma [3], vulvar neoplasms; - abscess of the Bartholin gland; - bartholinitis; vulvar abscess.
— Hematoma in the vulva area – there may also be complaints about a formation in the vulva area, discomfort during sexual intercourse, and pain. But when collecting anamnesis; and gynecological examination - the woman associates its appearance with mechanical trauma, childbirth; And the location is not in the area of projection of the large vestibular gland. [1]
— Paraurethral cysts – similar complaints. On examination - swelling in the paraurethral region (the area near the urethra) [1]
- Furunculosis of the labia majora. Complaints include formations in the perineal area, general malaise, hyperemia, edema, hyperthermia. Upon examination, the formation is localized in the area of the hair follicle and sebaceous gland. [1]
Surgical treatment of Bartholin gland cyst:
Treatment of Bartholin gland cysts is carried out without exacerbation of the inflammatory process. In this case, there are two options for surgical intervention: marsupialization of the cyst (creation of an artificial duct of the gland for the outflow of secretions) or extirpation (removal) of the Bartholin gland.
When performing marsupilization, the doctor opens the cyst capsule with a linear incision. The edges of the capsule are sutured with separate sutures to the edges of the skin wound, forming an external opening. A drainage tube or catheter is inserted to drain the contents of the cyst. After the operation, within two months, the external opening narrows, and a new excretory duct is formed.
Extirpation of the gland is carried out in case of recurrence of bartholinitis. To do this, a longitudinal incision is made on the inside of the labia minora. The gland is carefully isolated with a scalpel and removed, and catgut sutures are placed on the wound.
For any types of bartholinitis, after surgery and complete elimination of the inflammatory process, physiotherapy is prescribed on the 3-4th day - magnetic therapy and ultraviolet irradiation. All patients are advised to abstain from sexual intercourse until complete recovery, since there is a high probability of infection of the sexual partner. In order to prevent a relapse of bartholinitis, it is important to eliminate the cause of the disease, to completely recover from concomitant infections (chlamydia, gonorrhea, etc.), otherwise bartholinitis may occur again.
All patients must observe the following rules of personal hygiene:
- wash your face twice a day;
- wear comfortable underwear, preferably cotton;
- During menstruation, change pads and tampons every 3-4 hours to avoid re-infection.
During the recovery period, it is important to use drugs that enhance the immune system. These include vitamins, a balanced diet, and some herbal immunomodulators.
Treatment
Small, asymptomatic cysts may not be treated except for cosmetic purposes.
Often the clinician is tempted to simply incise the cyst or abscess because this technique may be effective for other common abscesses. However, simply puncturing a cyst or abscess of the Bartholin gland can lead to a relapse, since the edges of the tissues, when punctured or cut, very quickly close again due to the rapid healing or regeneration process [6]
Only large cysts, usually 3 or more centimeters, which interfere with daily activity and sexual life, and disrupt the aesthetic appearance of a woman’s external genitalia, are subject to surgical treatment.
The main goal of surgical treatment is organ-preserving - the formation of a canal and restoration of the function of the Bartholin gland,
Prevention of bartholinitis:
- regular visits to the gynecologist;
- protection against sexually transmitted infections - use of condoms, monogamous lifestyle;
- timely treatment of infections;
- strengthening the immune system: good nutrition, exercise, giving up bad habits.
In our clinic you can receive a full range of clinical and laboratory examinations before performing this surgical operation. The equipped operating room allows you to perform the operation both under local anesthesia and general anesthesia, with stay and observation in the ward for several hours.
Catheter placement – Word
This is a modern method of surgical treatment for Bartholin’s gland cyst, especially in case of its recurrence.
Under local anesthesia, the cystic area is opened with a small incision of about 5 mm, the contents are removed and sent for bacteriological examination, the cyst cavity is washed and a Word catheter is installed in it (this is a silicone tube 55 mm long, 5 mm in diameter with a channel inside, blindly ending, with thinner walls at the end, due to which the tip can inflate into a ball, which has no analogues), inflating its rubber tip to 3 ml with a physiological solution of 0.9% sodium chloride, thereby fixing it in the cavity of the cyst. For better fixation and prevention of loss during the woman’s movements, it is recommended to apply 2-3 absorbable interrupted sutures along the contour of the catheter emerging from the cavity of the cyst. The second end of the catheter is inserted into the vagina. The catheter remains in the cyst cavity for 6 weeks. This is aimed at forming a channel for the passage of secretions, the walls of which do not grow together. The study shows that the Word catheter is an easy-to-use, low-cost outpatient procedure with acceptable short-term recurrences. Treatment costs are seven times lower than with marsupialization [7]. While the catheter is in the cyst cavity, the patient is advised to have sexual rest to avoid its loss. In a number of countries there is no such restriction, since studies have shown that the pain symptom caused by both the cyst itself and the procedure performed with the catheter in the cavity completely disappears over time (by day 6) [8]
As an alternative, a Voroda or a Jacobi ring (the catheter does not have a channel, it is harder, shaped like a ring) which is installed through 2 punctures in the mucous membrane and capsule of the cyst and the 2 ends are fastened to each other.
VASCULAR FORMATIONS
Angiokeratoma
Angiokeratoma of Fordyce manifests as multiple, well-defined, bluish-black papules on the skin of the scrotum [Figure 7a]. They are often clinically mistaken for genital nevus, blue nevus and melanoma. Various sources indicate that 20% of angiokeratomas were misdiagnosed as melanoma [32]. Dermoscopy clearly shows pronounced reddish-dark blue lacunae with a blue-white veil [Figure 7B] [33].
Lymphangiectasia of the vulva
Acquired lymphedema and lymphangiectasia of the vulva usually occur due to damage to the lymph nodes that occur after trauma, infection, malignancy, surgery, radiation, etc. Clinically, they present as flesh-colored papules or transparent vesicles with a diffuse erythematous background. Piercing the lesion may release clear fluid. Dermoscopy reveals clearly defined, round-oval reddish lacunae with whitish septa and numerous small pinpoint lacunae. This is similar to the manifestations of lymphangioma. Dermatoscopy is relevant when lesions are sometimes confused with warts or molluscum contagiosum [34].
CONCLUSIONS
Dermatoscopy has become important in the diagnosis of non-pigmented dermatoses and for differentiating benign lesions from equivocal and malignant lesions [1, 28]. Many dermatologists in modern practice have included dermatoscopy in their routine work. Although this does not eliminate the need for biopsy, the technique avoids unnecessary biopsies of benign lesions. It also helps us carefully select the biopsy site for suspicious or atypical pigmented lesions.
BENIGN LOCATIONS
Seborrheic keratosis
Pigmented seborrheic keratosis, like its cutaneous counterpart, shows features such as polypoid structures, marrow-like structures, and finger-like structures on dermoscopy. Comedo-like structures, which are keratin-filled invaginations, are not observed in genital seborrheic keratosis due to constant friction. Milium-like cysts are usually visible because they are located intraepidermally [11,19].
Verruciform xanthoma
These are rare tumors composed of lipid macrophages that present clinically as yellowish plaques and nodules with a papillomatous surface in the anogenital areas. Dermoscopy reveals numerous yellowish papules with centrally located spiny vessels [20,21].
MALIGNANT EDUCATIONS
Melanoma
Vulvar melanomas account for 1-3% of all melanomas observed in women. They are often found in older women and present as flat or raised pigmented lesions that are often larger than 7 mm in size. Non-pigmented variants have also been described. Multiple colors and a multicomponent structure pattern characterize the dermoscopic picture of mucosal melanoma [11, 27]. The presence of blue, gray and white colors with or without structureless areas had 100% sensitivity for diagnosing melanoma [28]. Reticular depigmentation and a network of fine whitish lines are valuable in the diagnosis of early vulvar melanoma [10]. In non-pigmented melanoma, dermoscopy reveals whitish, skin-colored papules with polymorphic vessels [29]. Asymmetry, multicomponent patterns, blue-white veil, and the presence of vessels should raise suspicion of malignancy and be confirmed by histopathology [30].
Basal cell carcinoma
Dermoscopy of genital BCC is similar to cutaneous BCC, consisting of bluish-gray ovoid globules, whitish homogeneous areas, and tree-like vessels. Non-pigmented lesions are difficult to diagnose because... they can mimic inflammatory diseases. In this case, clearly visible tree-like vessels help make the diagnosis [31].
PRE-CANCEROR FORMATIONS
Extramammary Paget's disease
Extramammary Paget's disease is clinically characterized by erythematous plaques with oozing, ulcerated, and scaly nodules and focal hyperpigmentation. Areas of hypopigmentation can also be seen (Fig. 6a). Dermoscopy of extramammary Paget's disease reveals milky red areas, vascular structures, superficial scales, ulcers, pigment network, shiny white lines and white structureless areas [Fig. 6b]. Common vascular structures are stippled vessels and glomerular vessels [22]. Paget's disease is often mistaken for melanoma due to features such as irregular pigmented globules, white negative pigment network, and structureless blue-gray areas [23].
Erythroplasia Keira
It is the genital counterpart of Bowen's disease and has similar dermoscopic features. Glomeruloid vessels are characteristic, located in clusters or diffusely, which can be used to differentiate Queyre's erythroplasia from other causes of chronic balanitis. In addition, linear vessels and brown dots can be seen [24]. Dermoscopic features in pigmented Bowen's disease include pigmented streaks combined with other features such as comedo-like structures [25].
Vulvar intraepithelial neoplasia
This is a common cause of genital itching. About 15% of vulvar intraepithelial neoplasias are pigmented. Typical findings are milky white or pink areas associated with punctate or glomerular vessels and papillomatous structures. In the pigmented version, brownish dots with clearly defined boundaries and brain-like structures are visible [26].