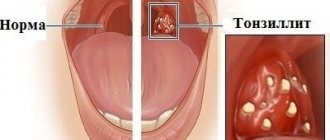
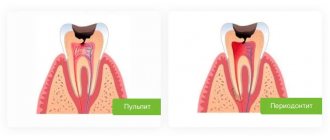
Gum cancer is included in the group of malignant neoplasms of the oral cavity along with carcinomas of the tongue, floor, cheeks and palate. Malignant processes in different anatomical structures of the oral cavity proceed differently, the reasons for their development and treatment methods are similar.
- Causes of gum cancer
- Stages
- Symptoms of gum cancer
- Risk group
- Diagnosis of gum cancer
- Treatment for gum cancer
- Prevention
- Forecast
- Possible complications of gum cancer
Causes of gum cancer
Statistics know the annual incidence of oral cancer - almost 9,300 Russians, but the number of patients with gum or tongue cancer is unknown. Processes that are close in localization are not similar in prognosis, for example, in terms of aggressiveness, “two big differences”: gum tumor behind the wisdom tooth and under the rest of the dentition, the common thing is the causes leading to malignant transformation.
Until the 2000s, tumors of the oral cavity were considered to be the property of alcoholics and heavy smokers, and cancer processes in this area were called “marginal.” Alcohol and tobacco abuse of all types - smoking or chewing - are still top of the list of risk factors today.
In the 2000s, the population of young and never-smoking intelligent patients leading a sober and healthy lifestyle increased sharply. It was clear that this cohort did not have a generally accepted root cause of cancer, and it was found - infection with human papillomavirus type 16. Unlike cervical cancer, which is also associated with HPV infection, oral carcinomas are not considered markers of promiscuity; a single encounter with HPV-16 is sufficient to initiate the disease.
Modern risk factors also include background processes in the mucous membrane - leukoplakia and erythroplakia, which are initially benign, but with a great potential for proliferation, which can lead to carcinoma in the distant future.
The third cause of gum cancer is chronic trauma to the mucous membrane from dentures, as well as a sluggish inflammatory process maintained by damaged parts of the tooth that are not removed in a timely manner.
Failure to comply with oral hygiene is also included in the causal list, although modern foreign scientists are skeptical about this factor, suggesting that all people brush their teeth twice a day. As targeted surveys and examinations of dentists show, in our country not all social groups have the same level of hygiene, and for Russians this reason is still relevant.
Unlike tumors of all other areas of the oral cavity, which men suffer from several times more often, gum cancer is not gender specific - both sexes are affected equally. The increase in incidence begins after 40 years of life, with each subsequent decade of life marked by a doubling of the number of cases.
Stages
In most cases, gum cancer is not detected at an early stage, which is typical for all oral tumors. People are not used to looking into their own mouth until there is a good reason for this - pain that occurs when the periosteum is involved in the process.
The height of the gum of an adult is small, however, when staging cancer, the tumor is graded in “steps” of 2 centimeters: less than 2 cm, from 2 cm to 4 cm, and more than 4 cm, because malignant processes of the oral cavity are often non-nodular. , and flat infiltrates and ulcers.
The stages of gum cancer are distributed as follows:
- stage 0 or carcinoma in situ - cancer cells have not penetrated into the deep layers of the mucous membrane, as a rule, the disease is visually manifested by leukoplakia, an oncological diagnosis is established only by microscopy;
- Stage 1 - carcinoma is less than 2 cm and there are no signs of damage anywhere else;
- Stage 2 - the primary lesion is more than 2 cm, but less than 4 cm, grows no more than a centimeter deep, there are no metastases in the lymph nodes;
- Stage 3 involves variability in the size of the primary gum lesion, including more than 4 cm, without metastases or with cancer cells in one lymph node no more than 3 cm in diameter;
- Stage 4 is divided into subgroups:
- 4A - extensive tumor without involvement of lymph nodes, or smaller in size with a large lymph node, but not more than 6 cm;
- 4C - the local condition is not important because there are distant metastases.
4B - cancer growing into the jaw and surrounding tissues without metastases, or a smaller lesion with large or multiple tumor lymph nodes on either side of the neck;
Tumors of the oral mucosa
SPECIALIZED ONCOLOGY CARE www.OncoClinic.com
Precancerous diseases
The development of cancer of the oral mucosa in 20-50% of cases is preceded by various precancerous diseases . Most often, precancer develops on the mucous membrane of the tongue (50-70%) and cheeks (11-20%). Processes with a high incidence of malignancy (obligate precancer) include Bowen's disease. Facultative precancers are represented by verrucous leukoplakia, papillomatosis, keratoacanthoma, erosive-ulcerative and hyperkeratotic forms of lupus erythematosus and lichen planus, post-radiation stomatitis.
Bowen's disease occurs more often in men aged 40-70 years, mainly in the area of the soft palate, uvula, and tongue. Clinically, it is characterized, as a rule, by the appearance of a single lesion in the form of a limited, slowly enlarging spotty-nodular lesion of a congestive red color measuring more than 1 cm in diameter. Its surface can be eroded and covered with small papillary growths. The diagnosis of the disease must be confirmed morphologically.
Verrucous leukoplakia differs from the flat form of leukoplakia by a greater degree of keratinization. The affected area of the mucous membrane protrudes above the surrounding tissues, its color is grayish-white, and there is a slight thickening upon palpation. Verrucous leukoplakia has plaque and warty clinical varieties. The warty variety has the greatest likelihood of malignancy. With this form, against the background of flat leukoplakia, dense-lumpy warty growths appear, which form mainly on the mucous membrane of the cheek, closer to the corners of the mouth.
Papillomatosis is characterized by the appearance of papillary growths on the mucous membrane. With the increased development of leukokeratosis, the surface of papillomatous growths acquires a whitish color. Inflammation often develops at the site of mucosal lesions. Superficial ulceration of the formation is possible.
Treatment of localized forms of precancerous diseases of the oral mucosa is surgical - excision, cryo- and laser destruction, electrical excision. Treatment of chronic ulcers on the oral mucosa includes the elimination of traumatic factors and conservative therapy. If there is no positive effect, a cytological examination of the prints or an excisional biopsy is performed within 2-3 weeks.
Cancer of the oral mucosa
The group of tumors of the oral mucosa includes malignant neoplasms of the mucous membrane of the tongue (excluding the root of the tongue), floor of the mouth, cheeks, hard and soft palate, alveolar process of the lower and upper jaw.
In the structure of incidence, cancer of the oral mucosa makes up 1.5% of the total number of malignant neoplasms. The highest rates are observed in southern and southeastern Asia, France and some countries in South America. The incidence of malignant neoplasms of the oral cavity in Russia (1997) is 2.7 per 100,000 population. In men, cancer of the oral mucosa develops 4-5 times more often than in women. Most patients are in the 5th-7th decade of life. The main factor contributing to the occurrence of cancer of the oral mucosa is smoking, which increases the risk of developing the disease by 2.5 times. When smoking and drinking strong alcohol are combined, the risk increases 15 times. Eating nasa and chewing betel leaves have a similar carcinogenic effect. Occupational hazards (prolonged contact with soot) and lack of vitamins B and A play a certain role. Other important etiological factors are chronic injuries and inflammatory processes of the oral mucosa.
The tongue (50-60%) and the mucous membrane of the floor of the mouth (20-35%) are most often affected by malignant tumors. Cancer of the buccal mucosa is observed in 8-10% of patients. It is extremely rare that tumors develop on the mucous membrane of the hard palate (1.3%). The vast majority of malignant neoplasms of the oral mucosa are represented by squamous cell carcinoma. A feature of its course is a tendency to lymphogenous metastasis to the superficial and deep lymph nodes of the neck (40-75%).
International histological classification of malignant tumors of the oral cavity and oropharynx
I. Tumors arising from stratified squamous epithelium:
1. Intraepithelial carcinoma (carcinoma in situ). 2.Squamous cell carcinoma. 3. Types of squamous cell carcinoma (verrucous carcinoma, spindle cell carcinoma, lymphoepithelioma). II. Tumors arising from soft tissues:
1. Fibrosarcoma. 2. Liposarcoma. 3. Leiomyosarcoma. 4. Rhabdomyosarcoma. 5.Chondrosarcoma. 6. Malignant hemangioendothelioma (angiosarcoma). 7. Malignant hemangiopericytoma. 8. Malignant lymphangioendothelioma (lymphosarcoma). 9. Malignant schwannoma. III. Tumors arising from the melanogenic system:
1. Malignant melanoma. IV. Tumors of controversial or unknown origin:
1. Malignant granular cell tumor. 2.Alveolar soft tissue sarcoma. 3. Kaposi's sarcoma. International classification according to the TNM system
T - primary tumor: Tx - insufficient data to evaluate the primary tumor, T0 - primary tumor not determined, Tis - preinvasive carcinoma (carcinoma in situ), T1 - tumor up to 2 cm in greatest dimension, T2 - tumor up to 4 cm in greatest dimension , T3 - tumor more than 4 cm in greatest dimension, T4 - tumor spreads to adjacent structures - bone, deep (external) muscles of the tongue, maxillary sinus, skin.
Notes:
1.The deep muscles of the tongue include the hypoglossus, genioglossus, and palatoglossus. 2. Superficial erosion of the osteodental cavity by a primary gingival tumor is not sufficient to designate the process as T4. 3. If there is doubt about the spread of the tumor to the bone, choose a less common category. If scintigraphy identifies a focus of pathological accumulation of radiopharmaceuticals, then the tumor is classified as T4. N/pN - regional lymph nodes: N/pNx - insufficient data to evaluate regional lymph nodes. N/pN0 - there are no signs of metastatic lesions of regional lymph nodes. pN0 - histological examination of material from a selected area of neck tissue includes 6 or more lymph nodes; histological examination of the material obtained using radical or modified radical lymphadenectomy includes 10 or more lymph nodes, N/pN1 - metastases in one lymph node on the affected side, up to 3 cm or less in the greatest dimension, N/pN2 - metastases in one or several lymph nodes on the affected side, up to 6 cm in greatest dimension, or metastases in the lymph nodes of the neck on both sides or the opposite side, up to 6 cm in greatest dimension: N/pN2a - metastases in one lymph node on the affected side, up to 6 cm in greatest dimension, N/pN2b - metastases in several lymph nodes on the affected side, up to 6 cm in greatest dimension, N/pN2c - metastases in lymph nodes on both sides or on the opposite side, up to 6 cm in greatest dimension, N/pN3 - metastasis in a lymph node more than 6 cm in greatest dimension.
Note. Lymph nodes on the affected side also include lymph nodes located in the midline.
M - distant metastases: Mx - the presence of distant metastases cannot be assessed, M0 - no distant metastases, M1 - distant metastases.
The requirements for determining the рТ category correspond to the requirements for determining the T category.
Grouping by stages
Stage 0 TisN0М0 Stage I Т1N0М0 Stage II Т2N0М0 Stage III Т3N0М0 Т1-3N1М0 Stage IVA Т4N0-1М0 Any ТN2М0 Stage IVB Any ТN3М0 Stage IVC Any ТAny NM1
Clinic. The anatomical forms of oral cancer are very diverse and do not have a generally accepted classification. Most often, cancer of the oral mucosa is a dense exophytic, easily bleeding neoplasm or ulcer with an uneven, tuberous bottom covered with a gray coating and raised edges, clearly demarcated from the surrounding tissues (ulcerative form). Sometimes an infiltrate is detected at the base of the ulcer, going deep into the tissue (ulcerative-infiltrative form). Tumors with an endophytic type of growth are more aggressive. The clinical course of oral cancer is divided into three periods of development. The early period is characterized by minor subjective unusual sensations of thickening of the mucous membrane, the appearance of a white spot of papillary neoplasms or a superficial ulcer, etc. As the tumor develops, it disintegrates, infection occurs, local pain of varying intensity occurs, salivation increases, and foul breath appears (advanced period). The period of neglect is characterized by rapid spread of the tumor to surrounding tissues, leading to significant impairment of the function of swallowing and speech.
Diagnostics includes examination and bimanual palpation, laryngoscopy, fiberoscopy of the oropharynx and nasopharynx, radiography of the facial skeleton (if indicated), morphological and cytological verification of the tumor, cytological examination of punctate enlarged lymph nodes. The clinical minimum examination includes chest x-ray and fibrogastroscopy (high probability of developing synchronous and metachronous damage to the mucous membrane of the upper respiratory and digestive tract).
When making a differential diagnosis, it is necessary to keep in mind nonspecific inflammatory processes, actinomycosis, tuberculous and syphilitic lesions of the oral mucosa, and goiter of the root of the tongue.
Prevention of oral cancer consists of timely treatment of precancerous diseases, sanitation of the oral cavity and rational prosthetics, elimination of bad household habits.
Cancer of the mucous membrane of the tongue
The predominant localizations of the tumor are the lateral edges of the tongue (72-84.4%) and the lower surface of the tip of the tongue (4-15%). The frequency of occurrence of the main clinical and anatomical forms of tongue cancer (exophytic, endophytic, mixed) is approximately the same. The vast majority of malignant tumors of the tongue are squamous cell carcinoma. In the anterior 2/3 of the tongue, cancer of the I-II degree of malignancy is more common; in the posterior third, carcinoma of the III degree of malignancy predominates. About 40% of patients at the time of treatment have clinically detectable metastases in regional lymph nodes. Cancer of the tip of the tongue most often metastasizes to the submental lymph nodes, and from there to the submandibular and deep cervical lymph nodes, cancer of the lateral surface of the tongue - to the submandibular and middle deep lymph nodes of the neck. When the tumor is located at the tip of the tongue or along the midline, bilateral metastasis is observed (5-20%). The biological aggressiveness of malignant tumors of the tongue is reflected in high rates of latent metastasis (30-40%).
Treatment . For stage I cancer of the movable part of the tongue, the surgical method is effective. For tongue cancer of stages II-III with an infiltration depth of no more than 4 cm without deep transfer of the tumor to the mucous membrane of the alveolar process of the mandible, the method of choice is combined radiation therapy. During implantation of intrastats, the issue of applying a temporary tracheostomy should be decided (high risk of tongue swelling and asphyxia). In other cases, treatment is combined. Remote gamma therapy is carried out in the preoperative period (SD 40-45 Gy). The irradiation field includes the primary focus and the area of stage I regional lymph nodes (in the absence of metastases) or all lymph nodes of the neck (in the case of clinically detectable metastases). The interval between the end of radiation therapy and surgery should not exceed 2-3 weeks. Hemiglossectomy is performed when the tumor diameter is no more than 4 cm using the electrosurgical method. Locally advanced tumors of the tongue are an indication for combined or extended operations. To perform combined operations, approaches through the mouth are used, with additional dissection of the tissues of the cheek or lower lip along the midline and various types of osteotomy. In case of advanced tongue cancer, the volume of resection is increased due to partial removal of the root and the opposite part of the tongue (subtotal and total glossectomy), all muscle structures of the tumor-affected area, the contents of the submandibular (required) and mental (if indicated) triangles. The spread of the tumor to the lower jaw is an indication for its segmental resection. In this case, it is necessary to apply a temporary tracheostomy and provide enteral nutrition to the patient. Total glossectomy or intersection of both hypoglossal nerves leads to the need for long-term tube feeding of the patient or the application of a gastrostomy. To improve functional and cosmetic results in penetrating resections of the mandible, vascularized complex bone-soft tissue free flaps, titanium implants, pedunculated musculocutaneous regional flaps, and free bone grafts are used.
Postoperative irradiation is carried out in the presence of a residual tumor (R1-2) up to a total focal dose of 70 Gy (taking into account previously performed radiation therapy). The volume of irradiated tissue includes the bed of the removed tumor and areas of its local spread.
Since the frequency of latent regional lymphogenous metastasis of tongue cancer is high, prophylactic bilateral lymphadenectomy is performed 2-3 weeks after surgery on the primary lesion or after completion of a course of radiation therapy. In the presence of clinically detectable metastases, cervical lymph node dissection on the affected side is performed simultaneously with removal of the primary lesion. After 3-4 weeks, prophylactic lymphadenectomy is performed on the opposite side.
The main types of surgical interventions on the cervical lymphatic system are the Krile operation and fascial-sheath excision of the tissue of the neck. The Crail operation is performed in the presence of multiple or single non-displaceable metastases in regional lymph nodes. With this type of intervention, the tissue and lymph nodes of the mental, submandibular and lateral triangles of the neck are removed. The boundaries of excision are the midline of the neck, the clavicle, the anterior edge of the trapezius muscle, and the lower edge of the mandible. The fiber is removed along with the sternocleidomastoid muscle, internal jugular vein, accessory nerve, submandibular and lower pole of the parotid salivary gland. Fascial-sheath removal of neck tissue is performed for enlarged lymph nodes that are suspicious for metastatic lesions, as well as for single metastases that are not fused with adjacent anatomical formations. The principal feature of fascial-case lymphadenectomy is the preservation of the internal jugular vein, sternocleidomastoid muscle and accessory nerve.
The prognosis depends on the degree of infiltration and the presence of regional metastases. The five-year survival rate for stage I-II cancer is 50-70% and stage III-IV cancer is 15-30%. Local-regional relapses in tongue cancer lead to death in 60-70% of cases. The mortality rate from distant metastases is 15%, from primary multiple tumors - 20-40%.
Cancer of the mucous membrane of the floor of the mouth
Clinic . The clinical course of tumors of the floor of the mouth is characterized by early spread of the process to surrounding tissues (gums, periosteum of the lower jaw). In turn, the tissues of the floor of the oral cavity are infiltrated secondarily by malignant tumors of the tongue, gums, lower jaw, and submandibular salivary glands, which must be taken into account in the differential diagnosis. Tumor involvement in the lower jaw can be determined by palpation - fixation of the tumor to the lower jaw is one of the signs of involvement of the periosteum or bone growth in the process. The immobility of the tongue indicates deep invasion of the tumor.
The first lymphatic barrier to cancer of the mucous membrane of the floor of the mouth is the submandibular and jugular-digastric lymph nodes (level I and II). The submental lymph nodes are rarely affected. Clinically recognizable metastases in regional lymph nodes occur in 30-40% of patients, in 20% of cases hidden metastases are observed. Distant metastases occur in 10-15% of patients.
Treatment of small tumors (T1) can generally be carried out by transoral resection with a margin of 2 cm from the macroscopically defined tumor edges, cryodestruction or radiation therapy. A number of foreign clinics are currently studying the possibilities of electrochemotherapeutic and electrochemical treatment. For exophytic tumors of the mucous membrane of the floor of the mouth with an infiltration depth of no more than 3-4 mm, the method of choice is application radiation therapy. Interstitial radiation therapy as an independent method can be used in the treatment of clearly demarcated tumors (T1-2) with an infiltration depth of 2.5-3 cm (SD 60-70 Gy). In other cases, preference is given to combined radiation therapy with external gamma therapy at the first stage at a dose of 30-40 Gy (T1-2) or 40-50 Gy (T3). If tumor regression is less than 50%, treatment is completed with surgery. Treatment of radiosensitive tumors is completed with interstitial radiation therapy at a total focal dose of 30-50 Gy. For medium-sized tumors (T2) of the anterior part of the floor of the mouth and deeply invasive neoplasms, bilateral irradiation of the first lymphatic barrier is mandatory. Contraindications to combined radiation therapy are the involvement of bone, large vessels, trismus in the tumor process, the presence of regional metastases, and the inaccessibility of the tumor for the introduction of sources.
Treatment of tumors corresponding to T3-4 local spread is combined: resection in combination with pre- or postoperative irradiation (40-50 Gy). For locally advanced tumors of the mucous membrane of the floor of the mouth, combined and extended operations are performed. In this case, the external carotid artery is first ligated and a temporary tracheostomy is applied for 1-2 weeks. The volume of excised tissue is determined by the extent of the tumor process. The most typical operations are:
1.resection of the floor of the mouth with simultaneous resection of a third or half of the tongue in a single block; 2.resection of the floor of the mouth with simultaneous marginal resection of the alveolar edge of the lower jaw or resection of the inner part of the lower jaw, to which the tumor adjoins; 3.resection of the floor of the mouth with simultaneous through resection of the lower jaw; 4. similar operations with simultaneous excision of the cervical tissue in a single block. Large postoperative soft tissue defects are eliminated with skin autografts, local flaps, and regional musculocutaneous flaps on a pedicle. In some cases, transplantation of complex tissue complexes (musculocutaneous, musculoskeletal, etc.) using microsurgical techniques is required. For through resections of the lower jaw, primary or delayed bone grafting or endoprosthesis replacement with titanium structures is indicated. If the continuity of the lower jaw is not restored simultaneously with the removal of the tumor, it is necessary to fix the bone fragments with special splints.
For stage I-II cancer, if there are no clinically detectable metastases and it is possible to regularly examine the patient, you can refrain from prophylactic regional lymphadenectomy. In common forms of the disease (stages III-IV), preventive irradiation of regional lymph nodes is indicated, which is carried out simultaneously with irradiation of the primary lesion, or bilateral cervical lymph node dissection. Fascial-sheath lymphadenectomy is performed 3-4 weeks after completion of treatment of the primary lesion. The treatment tactics for established regional metastases are similar to those for tongue cancer.
Drug treatment for cancer of the oral mucosa is used as neoadjuvant chemotherapy or for palliative purposes as part of chemoradiotherapy. The following combinations of drugs can be used:
1.cisplatin - 100 mg/m2 intravenously on day 1, fluorouracil - 1000 mg/m2 intravenously on days 1-4 with cycles every 3-4 weeks; 2. methotrexate - 40 mg/m2 intravenously on days 1 and 15, bleomycin - 10 mg/m2 intravenously on days 1, 8 and 15, cisplatin - 50 mg/m2 intravenously on day 4, with cycles every 3-4 weeks. If chemotherapy is insufficiently effective, monotherapy with taxanes or polychemotherapy using taxanes can be performed (taking into account cross-resistance to previously used drugs).
Treatment results depend on the size of the primary tumor, the presence of regional metastases, the degree of damage to the lower jaw and the radicality of the operation. According to summary literature data, the five-year survival rate for localized stage I-II tumors of the floor of the mouth is 60-80%. If the tumor crosses the midline of the fundus or spreads to the tongue and lower jaw, the five-year survival rate is within 50-60%, for tumors of stages III-IV - less than 50%. The presence of regional metastases reduces its rates to 25%.
Cancer of the mucous membrane of the gums and cheeks
Gum tumors are most often (80%) localized in the lower gum area behind the small molars. Exophytic neoplasms are more often papillary or verrucous and in the initial period of development may be similar to benign hyperkeratosis. Regional metastasis is observed in 15-30% of cases with cancer of the gum mucosa, and is less common with tumors of the cheeks. Latent metastases are detected in 10-20% of patients.
Treatment. Small superficial gum tumors can be treated with surgery or radiation therapy. When bone is involved in the process and large tumors (T3-4), combined treatment is performed (external gamma therapy + surgery). The volume of irradiated tissue includes the primary lesion and cervical lymph nodes on the affected side. Preventive irradiation of the lymph nodes of the neck is limited to the level of the first regional barrier. 2-3 weeks after completion of radiation therapy, segmental resection of the upper or lower jaw is performed. If there are metastases in the lymph nodes, cervical lymph node dissection on the affected side is performed simultaneously with excision of the primary tumor.
The spread of the tumor to the mucous membrane of the cheek and floor of the mouth is an indication for combined operations. A prerequisite for extended operations when the tumor is localized on the alveolar process of the lower jaw is the removal of the contents of the submandibular triangle on one side in a single block with the primary lesion, in case of damage to the anterior parts of the alveolar part of the lower jaw - the mental triangle, in case of tumor spread to the anterior parts of the floor of the oral cavity - submandibular triangles on both sides.
Malignant neoplasms of the cheek of stages I-II can be cured by surgery or combined radiation therapy. At the first stage, external beam radiation therapy is performed to reduce the biological activity of the tumor and reduce its volume; at the second stage, contact or interstitial radiation therapy is performed. For superficial tumors, contact radiation therapy can be used as an independent treatment method. In other cases, treatment is combined. Surgery is performed 2-3 weeks after completion of preoperative radiation therapy. Surgical access is carried out by crossing the lower lip along the midline with the continuation of the incision into the submandibular region. The block of tissue removed includes the tumor with surrounding tissues, a fragment of the lower jaw and masticatory muscles (if they are involved in the tumor process), and the contents of the submandibular triangle. Tumor growth into the mandibular canal is an indication for removal of half of the lower jaw. The resulting defect in the mucous membrane, skin and bone is eliminated by one of the types of plastic surgery. Cervical lymph node dissection is performed in the presence of clinically detectable regional metastases. Preventive irradiation of the regional lymphatic system is not carried out.
Forecast. Survival rates for tumors of the gums and cheeks depend on the size of the tumor, bone damage, and the presence of regional metastases. The average five-year survival rate of patients with gum tumors ranges from 78% (for stage I) to 15% (for stage IV). The results of combined treatment when bone is involved are significantly better than with radiation therapy.
According to summary data, the five-year survival rate for stage I-II cheek cancer is 65-74%, stage III-IV varies from 20 to 30%.
Cancer of the mucous membrane of the retromolar triangle
Tumors arising in the retromolar triangle are rarely limited to the gingival mucosa; the process may involve the nearby mucous membrane of the cheek, the anterior palatine arches, the floor of the mouth, and the back of the gums. A tumor of the retromolar triangle that extends to the anterior palatal arches may appear more similar in appearance to nasopharyngeal cancer.
The risk of clinically positive and latent metastases in the lymph nodes with these tumors is significantly higher than with gum tumors of other locations.
Treatment of superficial tumors, including those spreading to the soft palate and buccal mucosa, is radiation. If the periosteum is damaged, a partial (marginal) resection of the lower jaw is performed, even with small tumors. Moderately advanced and infiltrative tumors are treated in combination. At the first stage, surgical intervention is performed (resection of the lower jaw and cervical lymph node dissection), then external beam radiation therapy is performed. For locally advanced processes, treatment begins with preoperative radiation therapy, which in some cases allows the tumor to be transferred to a resectable state.
Cancer of the mucous membrane of the hard palate
On the hard palate, malignant tumors from the minor salivary glands (adenocystic carcinoma, adenocarcinoma) often develop. Adenocarcinomas tend to grow encapsulated for a long time. Rarely developing, squamous cell carcinoma tends to ulcerate quickly.
Treatment. The method of choice for treating squamous cell carcinoma without damage to the periosteum is intracavitary contact therapy (if it is technically possible to bring the stomastat to the lesion). In other cases, treatment is combined. At the first stage, preoperative radiation therapy is carried out, electrosurgical removal of the tumor is performed, retreating from the visible lesion of the mucous membrane by 3-4 cm. Postoperative defects are covered with obturating prostheses or eliminated using plastic surgery.
SIGN UP FOR A CONSULTATION by phone +7 (812) 951 - 7 - 951
Share link:
Symptoms of gum cancer
Gum tumors are divided into:
- exophytic - growing outward and forming a node;
- endophytic - spreading deep into the gums, in the form of a flat infiltrate or ulcer;
- mixed - a combination of two growth options; as a rule, this is a far advanced or recurrent process.
I detect a knot on the surface of the gum at an early stage, because it gets in the way, the tongue “feels” for it, and it gets injured when brushing your teeth or while eating. Infiltrates grow faster and are found later, when complaints of pain or bleeding appear.
Cancer in the initial stage does not hurt, especially since the oral mucosa is accustomed to irritating, spicy foods and hot foods. Temporary discomfort while eating does not cause everyone anxiety with a desire to see what is happening there. Gum cancer can masquerade as toothache, forcing you to see a dentist. Most often, it is the dentist who discovers the malignant process.
In stages 3-4, when cancer grows into the jaw, destroying the bone, the pain becomes constant, sharply intensifying while eating, and due to basic malnutrition leading to significant loss of body weight.
A large cancerous ulcer is accompanied by inflammation of the surrounding tissues and decay, causing intense pain radiating to the ear and temple. Secondary infection of the cancerous infiltrate is inevitable; it is manifested by a “heavy” putrid odor. The patient cannot open his mouth due to a painful spasm of the masticatory muscles - trismus. The general condition worsens, the temperature rises, and weakness increases.
Citizens who abuse alcohol drown out the pain by increasing the dose of alcohol, and complain of the appearance of a painful and often inflamed metastatic lymph node under the jaw or on the neck. The presence of various microflora in the mouth complicates metastatic conglomerates in the lymph nodes with secondary infection; when the size is more than 3-4 cm, a zone of decay is formed in the center of the lymph node, often with the formation of a fistula. During this period, symptoms of intoxication with high fever appear.
A reflex increase in salivation with impaired swallowing is characteristic. Salivation is very profuse, so it is possible that saliva may be thrown into the respiratory tract at night with the development of aspiration pneumonia. All malignant tumors lead to increased thrombosis and ease of development of bacterial infection in a weakened body. An additional negative factor is malnutrition up to complete starvation with exhaustion and the development of the fatal anorexia-cachexia syndrome.
Distant metastases are not typical for gingival carcinoma, but recurrences are common after treatment. Cancerous destruction of oral tissues with frequent bleeding from vessels destroyed by the tumor against the background of chronic inflammation in metastatic lymph nodes leads to a serious condition and death.
Risk group
Knowledge of risk factors allows you to calculate a likely “candidate” for the development of oral cancer and timely modify behavior towards a healthy lifestyle, eliminating actions that are hazardous to health.
High-risk group for malignant processes in the gum area:
- People who smoke have celebrated their fortieth birthday, because the frequency of neoplasms increases with age and the “control point”, after which the incidence doubles with each decade of subsequent life, is precisely 40 years.
- Young people with a full range of risk factors. Before the age of 40, carcinomas of this localization are rare, but early introduction to tobacco simultaneously with chewing betel or nas, with persistence in the mucosal cells of the human papillomavirus type 16, significantly increases the chances of cancer.
An extremely high-risk group when the prospect of becoming a cancer patient over time is very high:
- Suffering from precancerous processes - leukoplakia and erythroplakia;
- Older people who smoke, use dentures, and the older they are, the more likely malignant transformation is;
- Adults with a hereditary predisposition, which is identified by the presence in the family of patients with oral carcinomas.
All patients at risk should visit the dentist at least twice a year and undergo treatment for precancerous processes.
Removal of epulis on the gum
The need to remove the supragingival tissue occurs when the tumor is large, is growing rapidly, or is at risk of cancer. The procedure is complex and can only be performed by an experienced oral or maxillofacial surgeon.
Removal of epulis on the gum takes place under local anesthesia or sedation. The essence of the operation is to remove the lump and excise the affected tissue. Excision of the epulis itself can be done with a scalpel or laser. Dentists prefer a laser that can instantly stop bleeding and make precise “cuts.”
If the pathological process has penetrated deeply, it is possible to remove a section of bone using a cutter or bur. If teeth are damaged in the area where the tumor is located (loose teeth, exposed roots, etc.), the surgeon removes these teeth as well.
After the operation, the patient is covered with iodomorphic gauze. If there is a large area of dissection, the surgeon will apply sutures. A sterile bandage is applied over it.
In case of angiomatous and fibromatous appearance, removal of epulis on the gum can also be carried out if conservative therapy has not yielded results or the patient seeks help in the presence of complications.
Diagnosis of gum cancer
Oncopathology of the oral cavity is visual, that is, diagnosed during a routine examination without the use of any equipment.
During the initial examination, cells are scraped from the wound for cytological analysis, or, in the absence of an ulcer, the tumor is punctured with a thin needle. If possible, a part of the tumor is “bitten off” with a special instrument - this is a biopsy for histological analysis. The diagnosis of cancer is established solely by the result of a biopsy; cytology allows only to suspect the disease.
After morphological confirmation, an ultrasound of the oral cavity is performed, which explains the relationship of the neoplasm with the surrounding tissues, primarily with the bone and blood vessels, and the CT scan clarifies the condition of the entire anatomical region.
Next is the search for metastases: ultrasound of the neck, CT scan of the lungs or MRI.
Anatomical structure
The oral cavity is the initial section of the digestive tract, in which food is chewed and saliva is produced to digest food. It is involved in the process of breathing, swallowing, articulation and speech.
The composition of the oral cavity includes:
- vestibule (lips, front side of teeth, inner surface of cheeks);
- gums;
- the bottom on which the tongue lies;
- two thirds of the tongue;
- teeth;
- retromolar triangle - the space on the lower jaw behind the third molar;
- hard and soft palate.
Treatment for gum cancer
It is optimal to perform the operation at the first stage, if technically possible. The radicality of the surgical intervention ensures a distance of at least 2 centimeters from the tumor border; it is clear that this is possible with a small stage 1 lesion.
At stages 2-3, the possibility of surgery is limited by the depth of penetration of cancer cells deep into the tissues of the jaw; with a large depth of infiltration, the process is considered questionably operable, but a lot is determined by the experience and talent of the oncologist surgeon. Techniques have been developed that make it possible to replace large surgical defects of the jaw with skin flaps, ribs, metal structures or artificial tissues. Plastic surgery may be postponed until antitumor treatment is completed.
If the tumor thickness is more than 4 millimeters, the surgical plan includes removal of the lymph nodes of the neck; if the cancer infiltration is localized in the middle of the oral cavity, the nodes are removed from both sides. Lymphadenectomy has a positive effect on life expectancy, but reduces its quality. It is possible to refuse lymphadenectomy if there are no metastases, which is proven or rejected by a morphological study of a biopsy obtained from a “sentinel” lymph node.
Surgery for cancer above stage 1 is complemented by prophylactic radiation, which should begin one and a half months after surgery.
Initially inoperable stage 3 tumor conglomerates are tried to be reduced by radiation in combination with chemotherapy with platinum derivatives, postponing surgery to the second stage.
Contraindications for surgery: stage 4, proliferation of metastases from the lymph node into the skin or tissue of the neck, severe diseases in the decompensation stage.
If surgery is not possible, 7 weeks of radiation therapy is performed on the primary lesion and lymph nodes of the neck, with the introduction of platinum chemotherapy every 3 weeks. If radiation is contraindicated, chemotherapy is used; this is also done in case of relapse after chemoradiotherapy.
Discharge after surgery
Your surgeon will tell you when you can return to work and normal activities. It depends on the surgery you underwent and the speed of recovery.
In most cases, patients can cope with daily activities at home without additional help, but the nurse will discuss this with you before leaving the hospital. If you need help, your nurse or case manager can help arrange visits from a visiting nurse or home health professional.
Call your healthcare provider if you have any of these signs or symptoms of infection:
- temperature 101°F (38.3°C) or higher;
- increased redness around the incisions;
- increased discharge from the incisions;
- discharge that has an unpleasant odor;
- increased pain that does not go away after taking a prescribed pain reliever or acetaminophen (Tylenol®).
to come back to the beginning
Forecast
An individual prognosis for the course of the disease is based on the size of the neoplasm and the depth of its penetration deep into the jaw, involvement of vessels and nerves in the conglomerate.
The degree of damage to the lymph nodes affects life expectancy; metastases almost halve the likelihood of cure. Much determines the aggressiveness of cancer cells; low differentiation is not in favor of the patient.
Specific percentages by years of survival are unknown because the incidence is low and statistically gum cancer is not distinguished from the group of oral carcinomas.
Possible complications of gum cancer
First of all, patients are concerned about the cosmetic consequences of treatment; in this regard, chemoradiation treatment is preferable, but is fraught with a higher frequency of relapses and is inferior to surgery in terms of survival.
The list of dangerous complications of carcinoma includes deterioration in nutrition with exhaustion and the development of fatal anorexia-cachexia syndrome. Long-term cancer-preventive therapy worsens nutritional status and worsens underweight. From the first days of treatment, the patient necessarily needs nutritional correction and nutritional support with special protein mixtures. In some periods, the patient may require tube and parenteral nutrition, since swallowing is seriously impaired and spasm of the facial muscles develops, up to the inability to open the mouth due to trismus.
Malnutrition and tooth loss after irradiation worsen the course of concomitant diseases and contribute to the development of infections against the background of a natural decrease in immunity. A change in the swallowing reflex due to too intense production of saliva, literally flowing in a stream, leads to the night-time reflux of saliva with food debris and bacterial flora into the respiratory tract and the occurrence of severe aspiration pneumonia.
Blockage of lymph outflow and proliferation of neck vessels by metastatic lymph nodes is complicated by constant headaches and loss of consciousness.
The disintegration of a cancerous ulcer is fraught with bleeding, which can only be stopped by ligation of the artery. Tumor masses growing into the bones cause intense pain, aggravated by secondary infection. The most severe suffering for the patient's family is caused by the disintegration of a cancerous ulcer with the addition of a secondary infection and a foul odor. It is absolutely impossible to clear a progressive tumor of necrosis on your own; this is a very difficult task even for specialists.
Treatment of such patients is a great oncological art, which is available to the specialists of our clinic. We are ready to help any patient, with or without complications, who has been treated for a long time and is just beginning to fight for life.
Book a consultation 24 hours a day
+7+7+78
Bibliography:
- Alieva S.B., Alymov Yu.V., Kropotov M.A. etc. /Cancer of the oral mucosa. Oncology. Clinical recommendations // Ed. Davydova M.I.; M.: Publishing group RONC, 2015.
- Gelfand I.M., Romanov I.S., Udintsov D.B. /Tactics for the treatment of localized forms of cancer of the oral mucosa// Tumors of the head and neck; 2016; 6.
- Romanov I.S., Yakovleva L.P. /Issues of treatment of oral cancer// Farmateka; 2013; 8.
- Kurokawa H., Yamashita Y., Takeda S. et al. /Risk factors for late cervical lymph node metastases in patients with stage I or II carcinoma of the tongue// Head Neck; 2002; 24.
- Little M., Schipper M., Feng FY et al. /Reducing xerostomia after chemo-IMRT for head-and-neck cancer: beyond sparing the parotid glands// Int J Radiat Oncol Biol Phys; 2012; 83.
- Midgley AW, Lowe D, Levy AR et al. /Exercise program design considerations for head and neck cancer survivors// Eur Arch Otorhinolaryngol; 2018; 275(1).
Recovery
Throat cancer
During the recovery period, vitamin complexes with microelements are actively used. Vitamins A, B, C and D play an important role in the restoration of damaged tissues.
Physiotherapeutic procedures are used during the period of rehabilitation and regeneration and may include laser therapy, electrical myostimulation, inhalation and electrophoresis of medicinal substances, magnetic therapy, exercise therapy, and ultrasound therapy.